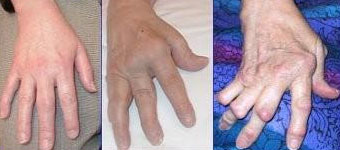
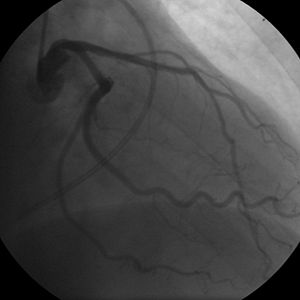
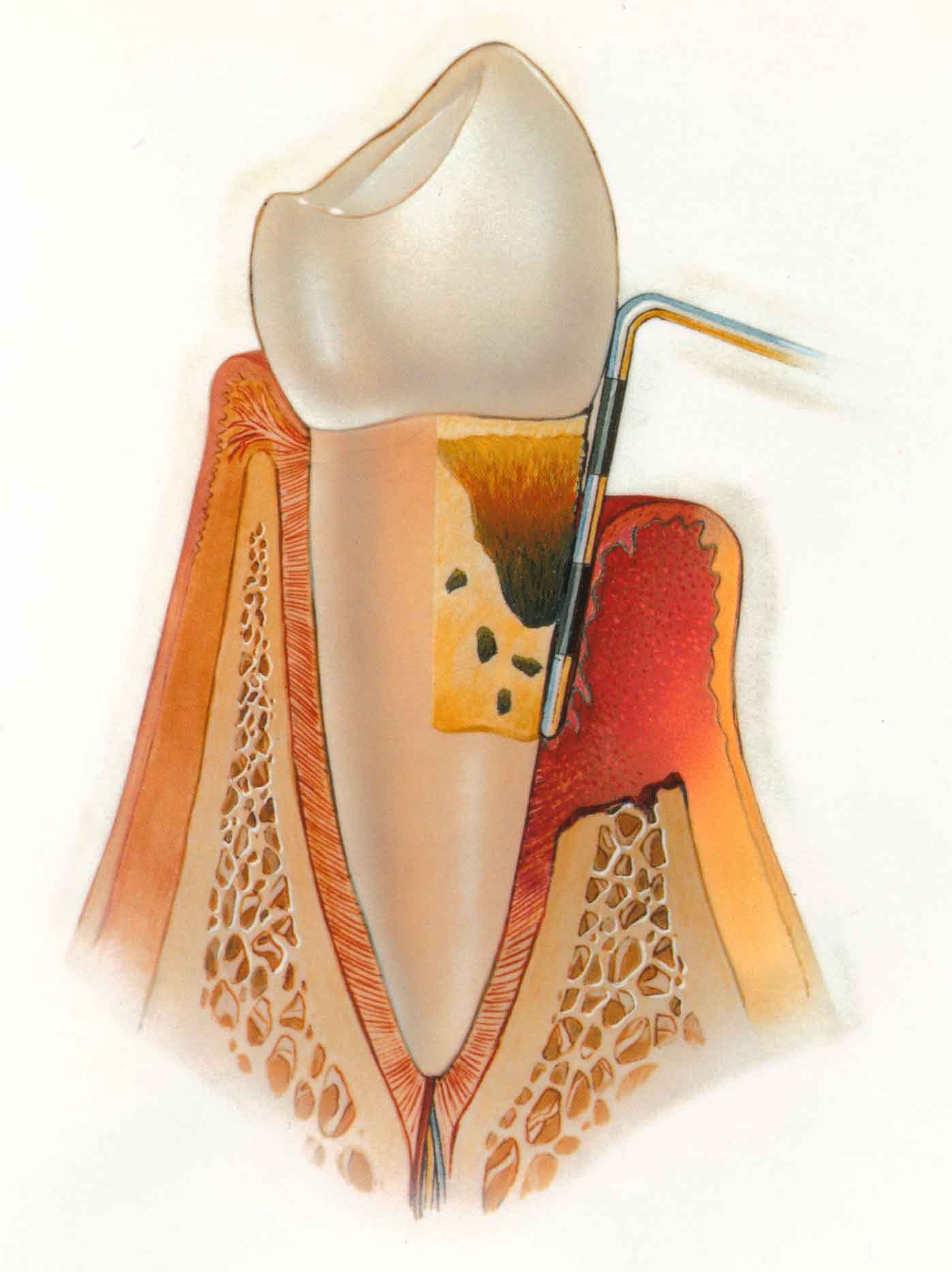
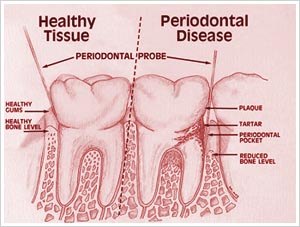
Arthritis is a complicated disease, which affects the joints of the body. There are more than a hundred different described conditions, with osteoarthritis and rheumatoid arthritis being the two most common ones. Osteoarthritis involves degeneration of the synovial cartilage and bony overgrowth on the joint articulating surfaces. Rheumatoid arthritis on the other hand has an autoimmune origin, involving self-production of auto-antibodies in the body which circulates in the blood and can attack the joints which are deemed foreign by the immune defense system. Although osteoarthritis and rheumatoid arthritis have different causes and risk factors, they are often present with similar symptoms, such as constant joint pain. Both diseases can be debilitating and adversely affect your oral health if not managed accordingly. Continue reading