The Hall technique is a novel method of managing carious primary molars by cementing preformed metal crowns, also known as stainless steel crowns, over them without local anaesthesia, caries removal or tooth preparation of any kind. Clinical trials have shown the technique to be effective, and acceptable to the majority of children, their parents and clinicians. The Hall technique is NOT, however, an easy, quick fix solution to the problem of the carious primary molar. For success, the Hall technique requires careful case selection, a high level of clinical skill, and excellent patient management. In addition, it must always be provided with a full and effective caries preventive programme.
The Hall technique will not suit every tooth, every child or every clinician. It can, however, be a useful and effective method of managing carious primary molars.
Background
The technique is named after Dr Norna Hall, a general dental practitioner from Scotland, who developed and used the technique for over 15 years until she retired in 2006. Preformed metal crowns (PMCs) have been used for restoring primary molars since 1950, and have become the accepted restoration of choice for the primary molar with caries affecting more than one surface, with a proven success rate as a restoration. Although popular with specialists, many clinicians find PMCs difficult to fit using the conventional approach, which requires the use of local anaesthetic injections and extensive tooth preparation. There is also an issue of potential damage to the adjacent first permanent molar when preparing a second primary molar for a PMC. For this, and
other reasons, PMCs are not widely used in the UK, forming less than 1% of all restorations provided for children.
How does the Hall technique get around some of these problems?
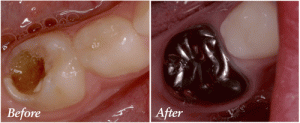 With the Hall technique, the process of fitting the crown is quick and non-invasive. The crown is seated over the tooth with no
With the Hall technique, the process of fitting the crown is quick and non-invasive. The crown is seated over the tooth with no
caries removal or tooth preparation of any kind, and local anaesthesia is not required.
For decades, conventional teaching has been that all carious tooth tissue should be removed before
restoring the tooth, unless there is a high risk of pulpal exposure.
How can leaving all the caries in the tooth be acceptable?
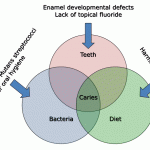
To answer this, it is worth firstly reviewing how and where caries begins. For many years it was assumed that all that was needed was to put a tooth surface, plaque and sugar together, add a little time, and caries would result. This combination can undoubtedly, under the right circumstances, cause caries, but what is remarkable is that so few tooth surfaces seem to be susceptible to carious attack. Clinicians will be aware that, except in extreme cases, the majority of tooth surfaces are
relatively immune from caries, despite many of these surfaces often having prolonged coverage by
plaque; for example, the labial and buccal cervical margins of teeth as they approach the proximal surfaces.
In fact, almost all caries begins at sites which collectively make up only a tiny proportion of the total area of enamel available for colonisation; the base of fissures, and just below the contact
point of proximal surfaces. The enamel here is almost identical in composition to that of the labial surfaces, so why the
difference? What differs is the ecological niche provided for plaque maturation by the very sheltered environment of these surfaces. Once caries has caused cavitation of the tooth, the availability of sheltered surfaces suitable for plaque colonisation and maturation dramatically increases, and so the caries continues through the tooth.
This all points to cariogenic plaque, (as different from non-cariogenic plaque), being extremely sensitive to the changes in its environment. If the environment can be manipulated, plaque can lose its cariogenic potential.
Plaque is far from the bland, homogenous material it appears to the naked eye. Given time, and a stable environment,
plaque will mature into a complex, organised structure, with channels and pores. Its bacterial population will shift and change in composition, with symbiotic relationships developing between some species, while other species will be gradually squeezed out by
their neighbours. In the deeper layers, organic acids formed as a by-product of bacterial metabolism, will favour a shift in the bacterial composition from noncariogenic species such as Streptococcus oralis and Streptococcus salivarius to more cariogenic species such as the mutans streptococci and lactobacilli. Plaque has been described by Marsh as a “city of slimeâ€. This is a useful analogy because just as a city is a complex structure, whose smooth functioning can be interrupted by a change in the supply of any number of factors (water, oxygen, power, light), so can the cariogenic potential of plaque be altered by changing the supply of
carbohydrates, oxygen, or the pH.