White sponge nevus (WSN), also known as Cannon’s disease, Hereditary leukokeratosis of mucosa and White sponge nevus of Cannon, is an autosomal dominant skin condition. Although congenital in most cases, it can first occur in childhood or adolescence.
Characteristics
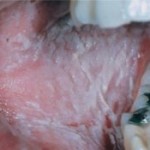
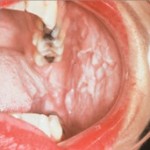
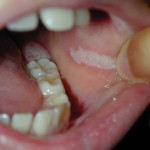
White sponge nevus almost always presents during childhood and there is no gender predilection. It presents in the mouth, most frequently as a thick bilateral white plaque with a spongy texture, usually on the buccal mucosa, but sometimes on the labial mucosa, alveolar ridge or floor of the mouth. The gingival margin and dorsum of the tongue are almost never affected. Usually asymptomatic, rare examples of mild discomfort have been reported from secondary infection.
Occasional lesions are less thickened and reveal a “watery” or semitransparent appearance. Lesions are usually well demarcated from the surrounding normal mucosa, as opposed to the poor demarcation of leukoedema and smokeless tobacco keratosis. The plaques do not change significantly when the cheeks are stretched and, rarely, the plaques are small, multiple and scattered about the affected mucosa rather than being a single more diffuse keratosis.
Although this condition is perfectly benign, it is often mistaken for leukoplakia. There is no treatment, but because there are no serious clinical complications, the prognosis is excellent.
Cause and genetics
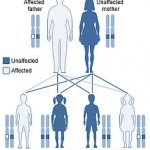
WSN is caused by a mutation of the keratin 4 or keratin 13 genes, located respectively at human chromosomes 12q13 and 17q21-q22. The condition is inherited in an autosomal dominant manner. This indicates that the defective gene responsible for a disorder is located on an autosome (chromosomes 12 and 17 are autosomes), and only one copy of the defective gene is sufficient to cause the disorder, when inherited from a parent who has the disorder.
Pathology and Differential Diagnosis
The hallmark microscopic feature of this disease is an extensive and often marked intracellular edema of the superficial epithelial cells, predominantly within the spinous layer. The nuclei are typically pyknotic and the cells may mimic the koilocytes of viral infections. Edematous cells may be organized into inverted triangles with broad bases along the surface, and there may be a thickened parakeratin layer. Deep indentations or groves may be seen to extend from the surface almost to the basal layer, but the lower portions of the epithelium are otherwise not involved. There are few mitotic figures and there is never evidence of dysplasia. In cytological smears occasional cells will have condensed eosinophilic cytoplasm immediately surrounding the nucleus.
Intracellular edema is not pathognomonic for white sponge nevus. Leukoedema is another developmental phenomenon with childhood onset and abundant superficial epithelial cells with edema. It typically lacks the parakeratosis and vertical groves of white sponge nevus, but there are times when the only viable means of distinguishing between the two is to stretch the affected mucosa; leukoedema tends to diminish or disappear when this is done, while no change is seen in white sponge nevus or other look-alike lesions.
Frictional keratosis, especially chronic cheek bite keratosis, may also present with intracellular edema of superficial epithelial cells, but there is usually extensive surface keratosis, vertical infolding is absent, and only occasional nuclei are pyknotic. Scattered chronic inflammatory cells are usually found within the subepithelial stroma.
Smokeless tobacco keratosis may demonstrate pronounced intracellular edema of superficial cells, sometimes extending to the parabasal region. It is also characterized by surface parakeratosis and occasional grooves or corrugations. This keratotic lesion may, therefore, exactly mimic the histopathology of white sponge nevus and may require clinical correlation for proper diagnosis. The smokeless tobacco lesion is white and corrugated, but its onset is associated with the smokeless tobacco habit and it is typically found in the mandibular vestibule, where the tobacco is habitually placed. Such lesions are, moreover, very seldom bilateral and they will usually disappear after cessation of the tobacco habit. It is important to differentiate these two entities because smokeless tobacco keratosis is a low-grade precancer and requires follow-up examinations.
 Another oral precancer, leukoplakia, is easily distinguished from white sponge nevus by its adult onset and its usual lack of intracellular edema. Leukoplakia is essentially a phenomenon of excess keratosis of the surface with acanthosis of the spinous layer and with occasional dysplasia of basal cells (see leukoplakia section elsewhere in this text).
Another oral precancer, leukoplakia, is easily distinguished from white sponge nevus by its adult onset and its usual lack of intracellular edema. Leukoplakia is essentially a phenomenon of excess keratosis of the surface with acanthosis of the spinous layer and with occasional dysplasia of basal cells (see leukoplakia section elsewhere in this text).
The final disease which may mimic the oral white macules of white sponge nevus is Witkop’s disease or hereditary benign intraepithelial dyskeratosis (HBID). The histopathology is identical to white sponge nevus except that scattered spinous cells demonstrate premature keratinization and loss or pyknosis of nuclei. This change is often seen as streaks of dyskeratotic cells. It is important for the pathologist to recognize this unique feature because persons affected by the autosomal dominant Witkop’s disease may develop gelatinous plaques of the bulbar conjunctiva which may eventuate in blindness.