In this article we will be discussing questions about osteonecrosis of the jaw such as :
What is it?
How does it happen?
What are the causes & risks for osteonecrosis of the jaw?
What are bisphosphonates?
Should I be concerned if I am on bisphosphonates?
Why is osteonecrosis of the jaw dangerous?
The treatment and prevention of osteonecrosis of the jaw will be further discussed in the article “Osteonecrosis of the Jaw Part 2”.
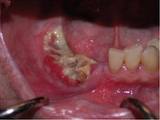
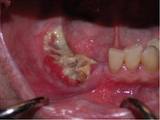
Osteonecrosis- exposed bone that does not heal in the right edentulous region of the lower jaw.
What is osteonecrosis of the jaw?
“Osteonecrosis†is made up of the words “osteoâ€, which means bone, and “necrosis†which means death of cells. Hence “osteonecrosis†of the jaw bone means death of cells in the jaw bones. It is diagnosed when an area of bone is exposed and shows no sign of healing or gum growing over it 8 weeks after an invasive dental procedure, such as tooth extraction or implant surgeries. Both the upper and lower jaw may be affected, and it may be associated with pain, numbness, swelling and infection of the affected site. The damage to the jaw bone is irreversible, and if left untreated, can spread and can cause devastating damages, even to the point of death. Continue reading →