Bisphosphonate-related osteonecrosis of the jaw (BRONJ) is a condition found in patients who have received intravenous and oral forms of bisphosphonate therapy for various bone-related conditions. Bisphosphonate-related osteonecrosis of the jaw (BRONJ) manifests as exposed, nonvital bone involving the maxillofacial structures. Bisphosphonate-related osteonecrosis of the jaw (BRONJ) is thought to be caused by trauma to dentoalveolar structures that have a limited capacity for bone healing due to the effects of bisphosphonate therapy.
Epidemiology
Frequency
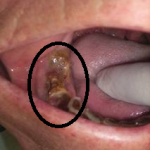
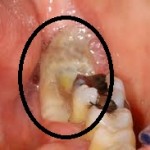
Biphosphonate induced osteoradionecrosis
The true incidence of bisphosphonate-related osteonecrosis of the jaw (BRONJ) has yet to be determined. The estimated incidence, according to a package insert in a special mailing by Merck Pharmaceuticals, is 0.7 per 100,000 persons per year.Most reports and experts disagree with this figure. Several recent studies of patients with multiple myeloma and patients with breast cancer who received intravenous aminobisphosphonate therapy for metastatic bone lesions demonstrated 6-11% of the patients developed bisphosphonate-related osteonecrosis of the jaw (BRONJ). The incidence of bisphosphonate-related osteonecrosis of the jaw (BRONJ) has been strongly correlated with the aminobisphosphonates pamidronate (Aredia) and zoledronic acid (Zometa) and is even higher in patients who have had recent dental extractions.
Kahn et al evaluated the association of osteonecrosis of the jaw with bisphosphonate use. Data that links the incidence of osteonecrosis of the jaw and its etiologic factors are limited, and the incidence of osteonecrosis of the jaw in the general population (ie, those not taking bisphosphonates) is unknown. Evidence is insufficient to confirm a causal link between low-dose bisphosphonate use in osteoporosis with osteonecrosis of the jaw. Osteonecrosis of the jaw is primarily associated with high-dose bisphosphonate use in cancer patients.
Etiology
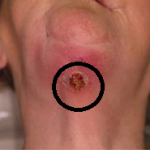 Bisphosphonate-related osteonecrosis of the jaw (BRONJ) is a condition in which bones of the maxillofacial skeleton, in particular the tooth-bearing areas, become necrotic and exposed to the oral cavity. Bisphosphonate-related osteonecrosis of the jaw (BRONJ) can be spontaneous, commonly appearing in the mylohyoid ridge area. Bisphosphonate-related osteonecrosis of the jaw (BRONJ) may also be caused by trauma, such as a tooth extraction or dental surgery. Exposed alveolar bone, which may be painful, is noted on examination.
Bisphosphonate-related osteonecrosis of the jaw (BRONJ) is a condition in which bones of the maxillofacial skeleton, in particular the tooth-bearing areas, become necrotic and exposed to the oral cavity. Bisphosphonate-related osteonecrosis of the jaw (BRONJ) can be spontaneous, commonly appearing in the mylohyoid ridge area. Bisphosphonate-related osteonecrosis of the jaw (BRONJ) may also be caused by trauma, such as a tooth extraction or dental surgery. Exposed alveolar bone, which may be painful, is noted on examination.
Pathophysiology
Bisphosphonates are believed to bind to osteoclasts and interfere with bone remodeling. They interfere with the cholesterol biosynthesis pathway by inhibition of farnesyl diphosphate synthase. In time, the cytoskeleton of the osteoclast becomes dysfunctional and the ruffled border needed for bone resorption is unable to form. Aminobisphosphonates have also been shown to have antiangiogenic properties. The overall effect is a decrease in bone turnover and inhibition of the bone’s reparative ability. Injury to the bone in these patients via tooth extraction, dental surgery, or mechanical trauma is thought to initiate bisphosphonate-related osteonecrosis of the jaw (BRONJ).
Presentation
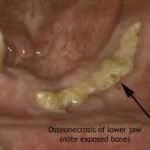 Symptoms may include the following:
Symptoms may include the following:
- Pain
- Swelling
- Cellulitis
- Halitosis
- Trismus
Physical findings may include the following:
- Mandibular and or maxillary bone exposure
- Pathologic fracture
- Oral-cutaneous fistula
- Clinical infection
Managing ONJ
The management of ONJ has yet to be finalized. Antibiotics, conservative debridements, irrigations and topical application of anti-infectives are seldom curative but may permit the patient to live with their disease. Hyperbaric oxygen does not seem to be effective. There are more advanced cases with patients who have responded poorly to conservative treatment that have required resection of the mandible or maxilla.
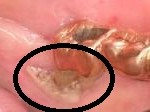 At this point, the best way to manage ONJ is to prevent it from occurring. There is a huge patient population taking bisphosphonate therapy and are at risk for ONJ, and many practitioners who are still unaware of this complication. The information is gradually getting out to treating physicians and dentists. Pharmaceutical companies have sent out letters to the oncologists and oral/maxillofacial surgeons, alerting them to this condition.
At this point, the best way to manage ONJ is to prevent it from occurring. There is a huge patient population taking bisphosphonate therapy and are at risk for ONJ, and many practitioners who are still unaware of this complication. The information is gradually getting out to treating physicians and dentists. Pharmaceutical companies have sent out letters to the oncologists and oral/maxillofacial surgeons, alerting them to this condition.
Patients currently taking bisphosphonates should be counseled to the risks of ONJ and be encouraged to seek dental care to optimize their oral health. Invasive dental procedures such as dental extractions and implant placement should be avoided if at all possible. Since bisphosphonate medications have half lives measured in years, stopping the medication for weeks or months will have little if any effect.
Patients who are planning bisphosphonate therapy should have a thorough oral exam and necessary work to eliminate all dental disease prior to the initiation of this therapy. The dental profession is accustomed to performing these pretreatment evaluations in high risk patients receiving head/neck radiation therapy, transplants, chemotherapy and heart valves, where dental complications in the post–treatment course can have signifi cant morbidity and even mortality.
Future outlook
 Currently, medical and dental practitioners, the pharmaceutical industry and government agencies are working to obtain additional information and provide answers as to the definitive management of this newly identified entity called ONJ. As practitioners, we must put ONJ on our radar screens when either treating pathology in the maxillofacial region or prescribing bisphosphonates so as to alert our patients to this possible complication of therapy. There is certainly more to come about bisphosphonate induced osteonecrosis of the jaws. We believe we are just seeing the tip of the iceberg.
Currently, medical and dental practitioners, the pharmaceutical industry and government agencies are working to obtain additional information and provide answers as to the definitive management of this newly identified entity called ONJ. As practitioners, we must put ONJ on our radar screens when either treating pathology in the maxillofacial region or prescribing bisphosphonates so as to alert our patients to this possible complication of therapy. There is certainly more to come about bisphosphonate induced osteonecrosis of the jaws. We believe we are just seeing the tip of the iceberg.