Other Treatments
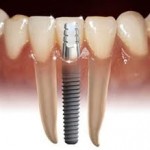
Dental Implants are used to replace missing teeth. Theoretically it is possible to do this successfully for a person with OI and there is anecdotal evidence that this has been accomplished. However, there are no controlled studies on the use of dental implants in people with OI and only a few case reports in the literature. The high failure, reported to be 50 per cent within 3 years of surgery is a concern.
Dental implants are somewhat like screws. In order to function, there must be enough bone in the jaw for the implant to be securely placed. After healing, a “post†is placed in the implant and an artificial tooth is attached. Good, strong healing around the implant is critical.
Veneers are cosmetic coverings typically placed on the outer surface of the upper anterior teeth. Anterior teeth are seen when a person smiles. Sometimes adults, often older children and especially adolescents with DI resent the color of their teeth. Adults can have veneers or crowns placed to change the appearance of the anterior “smiling teeth.†but older children and adolescents are too young to receive permanent restorations. They can be good candidates for composite veneers. Veneers can last for years and have the merit of being relatively inexpensive, versatile and are effective for hiding unsightly tooth color. However, veneers are not typically made to withstand biting forces. Recommendations for this type of treatment are made on a case by case basis.
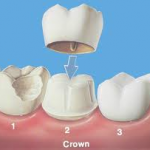 Caps and Bridges have a variety of uses. Caps, also called crowns, are made of metal or ceramic and cover the entire tooth after the enamel is removed. If teeth are wearing excessively, crowns usually provide the best treatment. Preformed stainless steel crowns are typically used for baby teeth, while cast metal or ceramic crowns are used for adult teeth. If there is not enough tooth left above the gum to place a crown, the individual may need gum surgery to make the part of the tooth showing above the gum larger. The surgeon may place a post down into the root of the tooth to act as a reinforcing rod, and then rebuild part of the tooth above the gum for the crown to sit on. In teeth not affected with DI, root canal treatment may be needed if the nerves and blood vessels inside the tooth are infected from a cavity or if the post needs to go down the center of the root(s).
Caps and Bridges have a variety of uses. Caps, also called crowns, are made of metal or ceramic and cover the entire tooth after the enamel is removed. If teeth are wearing excessively, crowns usually provide the best treatment. Preformed stainless steel crowns are typically used for baby teeth, while cast metal or ceramic crowns are used for adult teeth. If there is not enough tooth left above the gum to place a crown, the individual may need gum surgery to make the part of the tooth showing above the gum larger. The surgeon may place a post down into the root of the tooth to act as a reinforcing rod, and then rebuild part of the tooth above the gum for the crown to sit on. In teeth not affected with DI, root canal treatment may be needed if the nerves and blood vessels inside the tooth are infected from a cavity or if the post needs to go down the center of the root(s).
In teeth with DI, the inside where the nerves and blood vessels are normally located may already be filled with dentine. This makes placing a post in the center of the root and/or root canal treatment difficult, if not impossible. Small reinforcing pins may be placed in the dentine away from the center of the root to help make the new crown of the tooth stronger.
A bridge is at least one artificial tooth attached to one or more crowns. A bridge is sometimes called a fixed partial denture.
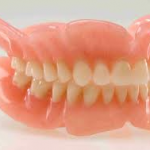
Complete Dentures are used when there are no teeth remaining in one or both jaws. How well the denture fits depends on how much bone remains after the teeth are lost. There are no studies that compare bone loss under dentures in people with OI to people without OI. The bone loss that occurs when teeth are lost is a resorption of the bone, not a fracture process, so it is not known if bone loss would be more rapid in people with OI. Complete dentures in children and adolescents who are still growing will need to be adjusted and or remade on a routine basis to compensate for growth in the jaw.
Removable Partial Dentures are used when some teeth remain in one or both jaws. A denture, typically made with a metal framework for strength and retention, is constructed to replace missing teeth.
Bisphosphonates
The class of drugs known as bisphosphonates is being used as a treatment for many bone disorders. An increasing number of children and adults with OI receive bisphosphonates as part of a clinical trial or on an “off-label†basis. These include: pamidronate (Aredia®) and zoledronic acid (Zometa®) given by intravenous infusion, and alendronate (Fosamax®), risedronate (Actonel®), and ibandronate sodium (Boniva®) given in tablet (oral) form. There have been reports in medical journals suggesting a link between bisphosphonates and areas of dead bone (osteonecrosis), particularly in the jaw.
Osteonecrosis could be caused by the type of bisphosphonate, the dose or the frequency of treatment. All of these factors are currently being studied. Even though at this time there appears to be no risk of bisphosphonate induced osteonecrosis of the bone (BON) associated with bisphosphonate therapy for OI, it may be prudent to take precautions. People with OI taking a bisphosphonate should be closely monitored by a doctor and a dentist. Good oral hygiene along with regular dental care to prevent infections or periodontal (gum) disease lowers risk. When possible, required dental surgery should be scheduled prior to starting bisphosphonate treatment. Bisphosphonate treatment should not be resumed until after the surgical area is healed. Elective jaw surgery, including dental implants, should be avoided during intravenous bisphosphonate therapy. Extraction of third molars (wisdom teeth) should be deferred until more information is available.
Bisphosphonates work by reducing the remodeling rate in the skeleton. In the short term, reduction of the remodeling rate produces bone with a greater density, although it is not clear if this results in greater strength. It is also not clear what impact this reduction in remodeling will have long term. Because the remodeling rates for bone surrounding teeth are typically higher than for other bones in the body, additional questions arise about the effect of bisphosphonates on the oral cavity. It is also not clear what effect bisphosphonates have on young children whose new teeth are erupting as they grow.
Similarly, the effect of bisphosphonates on the necessary remodeling surrounding dental implants is not understood. Separate from the concern about BON is the likelihood that tooth movement from orthodontia will decrease if the patient is taking, or has within some period of time, been taking bisphosphonates.