What is Clostridium difficile (C. difficile)?
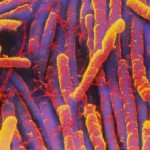
Clostridium difficile (C. difficile) is a bacterium that is related to the bacterium that cause tetanus and botulism. The C. difficile bacterium has two forms, an active, infectious form that cannot survive in the environment for prolonged periods, and a nonactive, “noninfectious” form, called a spore, that can survive in the environment for prolonged periods. Although spores cannot cause infection directly, when they are ingested they transform into the active, infectious form.
C. difficile spores are found frequently in:
- hospitals,
- nursing homes,
- extended care facilities, and
- nurseries for newborn infants.
They can be found on:
- bedpans,
- furniture,
- toilet seats,
- linens,
- telephones,
- stethoscopes,
- fingernails,
- rings (jewelry),
- floors,
- infants’ rooms, and
- diaper pails.
They even can be carried by pets. Thus, these environments are a ready source for infection with C. difficile.
What is Clostridium difficile (C. difficile) colitis?
 Antibiotic-associated (C. difficile) colitis is an infection of the colon caused by C. difficile that occurs primarily among individuals who have been using antibiotics. It is the most common infection acquired by patients while they are in the hospital. More than three million C. difficile infections occur in hospitals in the US each year. After a stay of only two days in a hospital, 10% of patients will develop infection with C. difficile. C. difficile also may be acquired outside of hospitals in the community. It is estimated that 20,000 infections with C. difficile occur in the community each year in the U.S.
Antibiotic-associated (C. difficile) colitis is an infection of the colon caused by C. difficile that occurs primarily among individuals who have been using antibiotics. It is the most common infection acquired by patients while they are in the hospital. More than three million C. difficile infections occur in hospitals in the US each year. After a stay of only two days in a hospital, 10% of patients will develop infection with C. difficile. C. difficile also may be acquired outside of hospitals in the community. It is estimated that 20,000 infections with C. difficile occur in the community each year in the U.S.
How does C. difficile cause colitis?
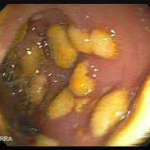
C. difficile spores lie dormant inside the colon until a person takes an antibiotic. The antibiotic disrupts the other bacteria that normally are living in the colon and preventing C. difficile from transforming into its active, disease causing bacterial form. As a result, C. difficile transforms into its infectious form and then produces toxins (chemicals) that inflame and damage the colon. The inflammation results in an influx of white blood cells to the colon. The severity of the colitis can vary. In the more severe cases, the toxins kill the tissue of the inner lining of the colon, and the tissue falls off. The tissue that falls off is mixed with white blood cells (pus) and gives the appearance of a white, membranous patch covering the inner lining of the colon. This severe form of C. difficile colitis is called pseudomembranous colitis because the patches appear like membranes, but they are not true membranes.
Not everybody infected with C. difficile develops colitis. Many infants and young children, and even some adults, are carriers (they are infected but have no symptoms) of C. difficile. C. difficile does not cause colitis in these people probably because;
- the bacteria stay in the colon as non-active spores, and
- the individuals have developed antibodies that protect them against the C. difficile toxins.
What are the symptoms of C. difficile colitis?
Patients with mild C. difficile colitis may have:
- a low-grade fever,
- mild diarrhea (5-10 watery stools a day),
- mild abdominal cramps and tenderness.
Patients with severe C. difficile colitis may have:
- a high fever (temperature of 102°F to 104°F),
- severe diarrhea (more than 10 watery stools a day) with blood, and
- severe abdominal pain and tenderness.
Severe diarrhea also can lead to dehydration and disturbances in the electrolytes (minerals) in the body. Rarely, severe colitis can lead to life-threatening complications such as megacolon (markedly dilated colon), peritonitis (inflammation of the lining of the abdominal), and perforation of the colon.
CLINDAMYCIN IN THE TREATMENT OF DENTAL AND MAXILLOFACIAL INFECTIONS
Acute dental infections
The efficacy of clindamycin in dental infectionshas been investigated in 5 prospective, randomized controlled, clinical trials, and 1 retrospective study, mostly involving management of periapical abscesses. The clinical trials effectiveness was high, with success rates of 97%-100%. The dosage of clindamycin used in these studies was 600 mg/day (150 mg 4 times daily), except for the retrospective study, in which patients received 1200 to 2400 mg/day. In addition, the clinical improvement in pain, fever, and swelling occurred more rapidly in patients receiving clindamycin than in those given the control therapy (usually penicillin).
In practice, the recommended dosing for clindamycin ranges from 150 mg 4 times daily to 300 mg 4 times daily.
In vitro susceptibility tests included in the aforementioned studies demonstrated that the majority of isolates were inhibited by a clindamycin concentration of 1.2 mg/mL or less. Clindamycin inhibited 94%-100% of anaerobic clinical isolates with MIC \ 1.2 mg/mL and 90%-100% of aerobic isolates with MIC \ 1.0 mg/mL. A dose of 300 mg produces a 1.1 mg/mL concentration in gingival crevicular fluid (GCF) after 6 hours, well above serum concentrations (0.1 mg/mL).
Periodontal disease
Four trials involving patients with periodontal disease have shown long-term benefits in the treatment of refractory disease for clindamycin at a dosage of 600 mg/day for 7 days. The endpoints used were clinical features combined with microbiologic outcomes at 1 and 2 years. One study revealed that clindamycin was superior to tetracycline at follow-up after 1 year.