Periodontitis means inflammation of the supporting tissues of the teeth or also known as the periodontium. Periodontal disease can generally be divided into chronic, aggressive and necrotizing periodontal disease.
Chronic periodontitis can appear at any age but is most prevalent in adults. The disease is characterized by inflammation of the supporting structures of the teeth and loss of gum attachment due to destruction of the periodontal tissues. Prevalence and severity of the disease increase with age. The levels of chronic periodontitis can be classified as:
1)Â Â Â Â Â Slight or early periodontitis: There is progression of the gum inflammation into the bone and early bone loss (less than 30%) is seen, resulting in slight gum attachment loss of 1 to 2mm with gum pockets depth of 3 to 4mm.
2)Â Â Â Â Â Moderate periodontitis: A more advanced state of the previous condition, there is increased destruction of tooth supporting structures, gum attachment loss up to 4mm, moderate to deep gum pockets (5 to 7mm), moderate bone loss (30 to 50%), loose teeth and exposure of roots of teeth.
3)Â Â Â Â Â Severe or advanced periodontitis: There is further progression of periodontitis with severe destruction of the tooth supporting structures, gum attachment loss over 5mm, increased bone loss (more than 50%), increased gum pocket depth (usually 7mm or greater), increased tooth movement and severe exposure of teeth roots.
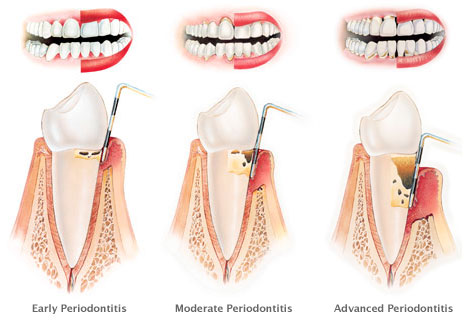
Levels of chronic periodontitis © Stanley Dentistry
Chronic Periodontitis symptoms
Chronic periodontitis has typically minimal symptoms but the disease is the chief cause of tooth loss in adult life. Many are unaware of the disease until their teeth become loose.
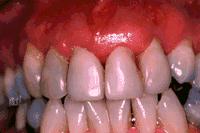
Chronic gingivitis (inflammation of the gums) is the initial stage of chronic periodontitis but having gingivitis does not necessary lead to periodontitis given that you have good oral hygiene. Some may complain of bleeding gums or an unpleasant taste if gingivitis persists. Later on, gum recession or teeth loosening becomes obvious. The gum margins become purplish-red, swollen and flabby and the gum tissues between the teeth gets destroyed leaving gaps in between teeth. Bleeding from the gum margins can occur when pressure is applied on it and sometimes pus can ooze out from the gum tissues at the necks of the teeth. Periodontitis is also a common cause for bad breath.
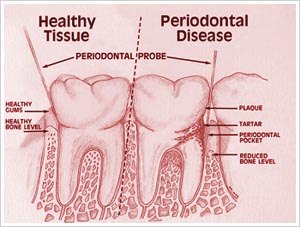
© Topnews.in
Destruction of the supporting structures of the teeth leads to:
- Loosening of teeth
- Deep pockets formation on the gums with tartar (calculus) felt inside
- Loss of attachment of the gum tissues to the teeth
- Bone loss which can be seen through X-rays
Cause of chronic periodontitis
Dental plaque is the major cause of periodontitis. Persistent infection of the gum margins leads to progressive inflammation and destruction of the supporting tissues by bacterial toxins and enzymes. Extension and the hardening of plaque leads to formation of tartar beneath the gums. Having tartar within the gum pockets can lead to periodontitis. It forms a reservoir of bacteria which help to keep inflammation and acts as a barrier to healing. The following risk factors can increase the chances of having periodontitis:
Risk factors for periodontal disease
Local factors
- Alignment and the bite relationship of teeth
- Faulty fillings of teeth
- Mouth breathing
- Dentures or braces
- Smoking
Systemic factors
- Diabetes mellitus
- Pregnancy
- Nutrition deficiency
- Blood diseases
- Drugs
- HIV infection
To be continued in the next part
Read about another type of periodontitis – apical periodontitis here.
Pingback: Does Mouth Wash really work? | Intelligent Dental
Pingback: Avoiding Trench Mouth | Intelligent Dental
Pingback: 10 Ways to Stop Bad Breath | Intelligent Dental
Pingback: Causes of Red, White or Pigmented Gums | Intelligent Dental
Pingback: Chronic Adult Periodontitis: Treatment and Prevention | Intelligent Dental
Pingback: Are You Brushing Your Teeth Away? | Intelligent Dental
Pingback: Are Dental Veneers for You? | Intelligent Dental
Pingback: Which is the Best Mouthwash for Gingivitis? | Intelligent Dental
Pingback: Deciding for ceramic dental implants | Intelligent Dental
Pingback: Apical Periodontitis: Symptoms and Treatment | Intelligent Dental
Pingback: How Diabetes Can Affect Your Oral Health Part 2 | Intelligent Dental
Pingback: Reasons to do a gingival flap surgery | Intelligent Dental
Pingback: How to Recognize Gingivitis Symptoms | Intelligent Dental
Pingback: Which Vitamins are essential to cure Gingivitis and reverse its damage | Intelligent Dental