What is Thalassemia?
Hemoglobin is the protein found in red blood cells in our blood that is responsible for carrying oxygen to all the different parts of out body. Hemoglobin is made up of 4 protein chains, ie 2 beta globin and 2 alpha globin. Thalassemia occurs when there is decrease in production or absence of production of either of these chains, leading to malfunctioning hemoglobins that are unable to carry oxygen. This then leads to anemia.
Thalassemia is thus classified by the type of globin that is affected: either alpha thalassemia or beta thalassemia, and each is classified according to the severity of which one is affected, ie either thalassemia major or thalassemia minor. People with thalassemia minor, either alpha or beta, may not have any symptoms.
Thalassemia is an inherited disorder, and is inherited as an autosomal recessive. This means that in order for a child to be thalassemic, both genes that the child received from his or her parents (one from each parent) carry the genes for thalassemia.
Symptoms of thalassemia patients:
1. Thalassemia patients have overactive bone marrow that leads to enlarged and thickened head and face bones. This can lead to deformities of the head and face. For example, the upper and lower jaws are larger than normal. This can lead to problems such as:
i) Malocclusion
ii) Enlarged tongue (macroglossi)
iii) Child patients have the same normal tooth size as other children. However, due to faster rate of growth of the jaw, there may be spacing between their teeth, leading to unsightly appearance.
– They also have the tendency to have weak arms and legs that fracture easily.
2. Iron overload
The treatment for more severe thalassemia is through blood transfusions or bone marrow transplant. Regular blood transfusions can lead to iron overload, which can then lead to cardiac failure, or affect liver and endocrine system. Hence patients undergoing blood transfusion also take iron-chelating agents (such as Desferron) after transfusions to remove excess irons from the body. Desferron can be deposited on skin, thus why some of the thalassemic patients have a grayish appearance of skin.
3. Other symptoms of anemia such as shortness of breath, fatigue and pallor.
4. Shortened life span
-Those with thalassemia minor usually have a normal lifespan, but patients with thalassemia major often have their life shortened due to complications such as heart and liver failure.
Diagnosis
Thalassemia can be diagnosed through the following methods:
i) Blood test (Full blood Count)- A full blood count (FBC) will show decreased red blood cell counts and hemoglobin level in patients with more severe thalassemia. However, a decrease in rec blood cell counts does not necessarily mean that the patient is thalassemic. Iron levels can be determined in order to rule out iron defeciency anemia.
ii) DNA testing- This is useful in testing for presence of the mutated gene that causes thalassemia.
iii) Prenatal genetic testing- Blood of fetus can be taken to test for thalassemia. Amniotic fluid may also be used, and is the preferred method as it causes less harm to the fetus. However, the parents should be fore-warned that any prenatal genetic testing carries the risk of miscarriage.
Consideration during dental treatment
1. Any dental treatment plan should first be discussed with the hematologist.
2. No dental treatment should be attempted when the hemoglobin level is low. As thalassemic patients go for regular blood transfusion, the timing of treatment should be adjusted accordingly, ideally soon after a blood transfusion.
3. Antibiotic cover is necessary for patients who have undergone splenectomy and requiring invasive dental treatment. These antibiotic should be able to reach the bone, such as Unasyn (a penicillin + sulbactam), clindamycin and tetracyclin. However, tetracycline is contraindicated in children as it can cause intrinsic staining of teeth during the developmental stage of the permanent teeth.
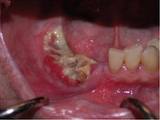
Osteoradionecrosis of the lower jaw
4. Due to weakened bones, these patients may be taking bisphosphonates (eg. Fosamax). Bisphosphonates can cause osteoradionecrosis of the jaw, which is none-healing of jaw bone. This becomes dangerous when an extraction is done and the bone does not heal but undergoes necrosis (cell death). This necrosis can spread, and if left untreated, can be fatal. It is therefore crucial for such patients to take extra care of their dentition to prevent the need of an extraction. This can be achieved through:
-emphasis on oral health education from young
-change in diet/nutrition
-Tooth Mousse is highly recommended as it can reverse early caries formation.
-fissure sealants
-routine dental checkup (6 monthly)
5. If an orthodontic treatment is done in such children, tooth movement occurs at a faster rate than would a normal child, hence movement of teeth should be monitored more closely.
6. Any dental procedures should be done in as little time as possible to avoid fatigue and reduce anxiety of such patients.