 What is a dry socket?
What is a dry socket?
Dry socket or also known as alveolar osteitis is a common complication occurring after the extraction of a permanent teeth especially the lower wisdom teeth. The term ‘alveolar’ refers to the jawbone that supports teeth while ‘osteitis’ refers to the inflammation of the bone associated with the extraction socket.
The condition has generally been characterized by degraded or delayed healing associated with breakdown or dislodgement of the blood clot in the extraction socket. It is usually accompanied by persistent, radiating pain in and around the extraction site within a few days after extraction that is not easily relieved by pain killers. The premature loss or breakdown of the blood clot is accompanied by exposure of the underlying bone.
 Signs and symptoms of dry socket
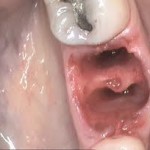
Signs and symptoms of dry socket
- Presence of postoperative pain in and around extraction site that increases in severity at any point 1 to 3 days after the tooth extraction. The pain can spread to other facial and ear regions.
- A partially or totally disintegrated blood clot within the extraction socket or an empty socket with exposure of underlying bone which is very sensitive and painful.
- Presence of debris or foreign bodies within the socket.
- Redness of the gums around the socket.
- Presence of bad breath (halitosis).
- Unpleasant taste in the mouth.
- However, there is no fever or lymph node enlargement.
How does a dry socket occur?
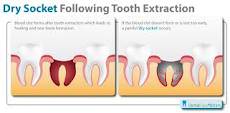 Normally, a blood clot forms at the site of a tooth extraction. This blood clot serves as a protective layer over the underlying bone and nerve endings within the socket. It also acts as a foundation for new bone growth and development of connective tissue.
Normally, a blood clot forms at the site of a tooth extraction. This blood clot serves as a protective layer over the underlying bone and nerve endings within the socket. It also acts as a foundation for new bone growth and development of connective tissue.
Dry socket occurs when the blood clot does not form completely, or it dissolves too soon or is physically dislodged before complete healing. Without the clot, new connective tissues and bone cannot fill in the socket and thus followed by the exposure of the underlying bone and nerve endings to the oral environment. This can cause intense pain, not only in the socket but also along the nerves radiating to the side of your face.
Factors that can increase your risk of developing dry socket
- Excessive surgical trauma during difficult extraction.
- Excessive use of vasoconstrictor in the local anesthetic solution- vasoconstrictors reduce blood supply by narrowing blood vessels around socket.
- Smoking or tobacco use-Â ingredients may inhibit healing and contaminate the wound site; the act of sucking on a cigarette may physically dislodge the blood clot prematurely.
- Use of oral contraceptives– estrogen component apparently enhances blood clot disintegration
- Improper home care- failure to follow postoperative instructions like excessive mouth rinsing after tooth extraction.
- Use of perioperative corticosteroids and antibiotics– increased tendency to infection.
- Tooth or gum infection– current or previous infections around the tooth to be extracted increase the risk
- Medical conditions like bone pathologic features, radiotherapy, vascular or hematologicdisorders and diabetes mellitus- delay wound healing process
Treatment
Given the severe pain and subsequent anxiety of patients with dry sockets, pain relief is the primary goal of treatment. Hence, the treatment of dry socket is palliative, given that healing occurs eventually within 1 to 4 weeks postoperatively.
- Cleaning and irrigation of the extraction socket- to remove any debris and bacteria from the denuded bone.
- Medicated dressings like Alvogyl– to fill the gap in the socket, prevent the accumulation of debris, relieve the pain, disinfect the alveoli, promote healing as quickly as possible and prevent malodor emanating from the empty socket; The active components of most dressings possess antibacterial, analgesic or a topical anesthetic properties, or a combination of these characteristics. You may need to have the dressing changed several times depending on your symptoms.
- Recently, low–level laser therapy (LLLT) has gained considerable recognition- continuous-mode diode laser irradiation applied for 60 seconds perpendicular to a single point on the wound surface at a distance of approximately 1 cm; studies have shown that LLLT increases the speed and quality of wound healing and has an overall positive effect on the inflammatory processes.
- Self–care– you may be instructed to flush the socket at home to eliminate debris and promote healing until the socket does not collect anymore debris.
Prevention
What your dentist can do?
- Minimize trauma during tooth extraction with copious saline irrigation.
- The following medications may help prevent dry socket:
- Antibacterial mouth rinses or gels immediately before and after extraction.
- Oral antibiotics for those with compromised immune systems.
- Antiseptic solutions applied to the wound.
- Medicated dressings after extraction.
What you can do before surgery?
- If you take oral contraceptives, schedule your extraction, if possible, during days 23 to 28 of your menstrual cycle, when estrogen levels are lower.
- Stop tobacco use at least 24 hours before extraction.
- Inform your dentist about any medications or drugs being consumed as some of them may interfere with blood clotting.
What can you do after surgery?
- Food– Avoid hard, sticky, hot or spicy foods that might get stuck in the socket or irritate the wound.
- Beverages– drink lots of water; avoid alcoholic, caffeinated, carbonated or hot beverages 24 hours after surgery; don’t drink with a straw as the sucking action may dislodge the clot in the socket.
- Oral hygiene– must be maintained wherever possible; brush all non-tender areas regularly and rinse with warm salt water 24 hours after surgery
- Tobacco use– if you smoke, don’t do so for at least 24 hours after surgery; if you chew tobacco, don’t use it for at least a week?
Alveolar osteitis or dry socket is the condition occuring after tooth extraction when the clot gets dislodged due to one or the other reason. It requires immediate consultation of dentist. It is most commonly seen during wisdom tooth extraction. It is usually treated with gauze mixed with ZOE. Visit for more info : http://www.identalhub.com/dental-what-is-dry-socket-879.aspx