Desquamative gingivitis is a cutaneous condition characterized by diffuse gingival erythema with varying degrees of mucosal sloughing and erosion.
A band of red atrophic or eroded mucosa affecting the attached gingiva is known as dequamative gingivitis. Unlike plaque-induced inflammation it is a dusky red colour and extends beyond the marginal gingiva, often to the full width of the attached gingiva and sometimes onto the alveolar mucosa. DG is more common in middle-aged to elderly females, is painful, affects the buccal/labial gingiva predominantly. Some reserve the term for cases where the epithelium blisters or peels while others use it whenever the characteristic red appearance is present. (Edward W. Odell, 2010)
What causes desquamative gingivitis?
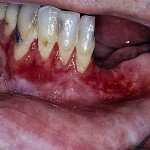 The top layer of the gum attaches to the lower layers through connective tissues. This condition causes the connective tissues to atrophy. This allows the upper layer to peel away. It often affects only patches. As a patch pulls away, it forms a blister. The exact cause of desquamative gingivitis is unknown. However, the presence of excessive bacteria in the mouth can aggravate it severely. The bacteria get into the space between tissue layers and cause infection. This leads to worse problems.
The top layer of the gum attaches to the lower layers through connective tissues. This condition causes the connective tissues to atrophy. This allows the upper layer to peel away. It often affects only patches. As a patch pulls away, it forms a blister. The exact cause of desquamative gingivitis is unknown. However, the presence of excessive bacteria in the mouth can aggravate it severely. The bacteria get into the space between tissue layers and cause infection. This leads to worse problems.
Common causes
- Lichen planus
- Mucous membrane pemphigoid
- Pemphigus
Gingival lichen planus
Desquamative gingivitis as a presenting feature is most commonly noticed in oral lichen planus (OLP).Lichen planus is a relatively common immunologically mediated mucocutaneous disease of unknown aetiology. It is more common in middle-aged to elderly females. Several forms of OLP are described intraorally; reticular, papular, plaque-like, atrophic, bullous and erosive forms. The most common site of involvement is the buccal mucosa followed by the tongue and the gingiva. The characteristic features of OLP are its chronicity, symmetrical appearance and multi-site involvement.
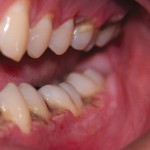 The gingiva may be the only site of involvement in about 10 per cent of cases. The atrophic form of OLPÂ presents often on the gingiva giving the classical appearance of DG. The whole thickness of the attached gingiva up to the mucogingival junction may be affected. The gingival tissues appear erythematous with occasional areas of erosions and possibly white striae at the periphery. Patients may complain of persistent soreness of the gums which is made worse by spicy foods or when carrying out daily oral hygiene procedures. The latter may become restricted to the point that plaque induced gingivitis and periodontitis sets in, confusing the clinical picture. However, it is important to note that the immunological reaction occurring in lichen planus does not result in clinical attachment loss and periodontitis.
The gingiva may be the only site of involvement in about 10 per cent of cases. The atrophic form of OLPÂ presents often on the gingiva giving the classical appearance of DG. The whole thickness of the attached gingiva up to the mucogingival junction may be affected. The gingival tissues appear erythematous with occasional areas of erosions and possibly white striae at the periphery. Patients may complain of persistent soreness of the gums which is made worse by spicy foods or when carrying out daily oral hygiene procedures. The latter may become restricted to the point that plaque induced gingivitis and periodontitis sets in, confusing the clinical picture. However, it is important to note that the immunological reaction occurring in lichen planus does not result in clinical attachment loss and periodontitis.
Diagnosis of OLP can be difficult if the gingiva is the only site of involvement. Careful examination of the erythematous gingiva may reveal faint keratotic lines. The rest of the oral mucosa should be examined carefully for evidence of classical lichenoid lesions. The patients should be questioned and examined for the presence of any cutaneous lesions. The most common cutaneous site involved in lichen planus is the flexural surface of the wrist, presenting as intensely pruritic, purple, polyglonal papules. Other sites that can be affected are the nails, scalp, oesophagus and the genital mucosa. In recent years, there have been reports of concomitant involvement of the genital mucosa and the gingiva, especially in females. This association of lichen planus of the vulva, vagina and the gingiva (presenting as classical DG) has been termed the vulvovaginalgingival syndrome.
An incisional biopsy is necessary to confirm the diagnosis of OLP. The biopsy should be taken well away from the marginal gingiva as plaque-induced
How can you treat desquamative gingivitis?
The underlying cause is unknown, so treating the symptoms is the way to go. Keeping infections in check means keeping the bacteria amounts reduced. The mouth plays host to almost two dozen bacteria regularly. When bacteria grow 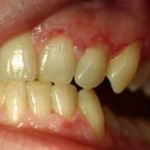 unchecked, they cause problems in a healthy mouth. In someone with this type of gingivitis, the bacteria cause massive infections that can destroy tissue. Reducing the amount of bacteria is vital to preventing these infections.
unchecked, they cause problems in a healthy mouth. In someone with this type of gingivitis, the bacteria cause massive infections that can destroy tissue. Reducing the amount of bacteria is vital to preventing these infections.
How do you reduce the amount of bacteria in the mouth?
For desquamative gingivitis sufferers, finding a solution is vital. The same remedies that prevent bacteria build up in gingivitis will help those that have desquamative gingivitis. The best remedies contain essential oils straight from nature’s drug store. These oils naturally prevent bacteria growth in the mouth. While eliminating bacteria in the mouth is impossible, it is possible to keep them in check. These remedies are anti-bacterial and anti-microbial. This gives the mouth time to heal and keeps the infections to a minimum. Help yourself with a natural remedy if you suffer from desquamative gingivitis. So there you have it. Find a natural way to keep bacteria in check.