EDEMA
Causes:
Trauma during injection
Injection of irritating solution
Infection, hemorrhage
Allergy (Angioedema)
Problems:
Pain & dysfunction
Airway obstruction
Prevention:
Proper care & handling of armamentarium
Atraumatic injection technique
Complete medical evaluation prior to injection
Management:
Trauma – resolve in few days without therapy
Hemorrhage – resolve slowly 7-14 days
Allergy – life threatening, airway impairment – basic life support, call medical help, Epinephrine – 0.3mg, Antihistamine, Corticosteroids
Total airway obstruction – Tracheostomy / Cricothyroidectomy
SLOUGHING OF TISSUES
Causes:
Epithelial desquamation
Sterile abscess
Problem:
Pain
Prevention :
Restricting use of topical anesthetics to 1-2 min.
Using less concentrated solutions
Management:
Symptomatic, Analgesics and topical ointment
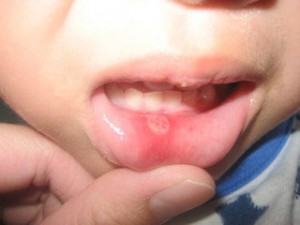
POST ANESTHETIC LESIONS
Patients report ulceration in the mouth almost 2 days after injection
Causes:
Recurrent aphthous stomatitis
Herpes simplex
Problem:
Acute pain in the area
Management:
Symptomatic, use topical anesthetics like viscous lidocaine, Benadryl, Orabase without Kenalog, tannic acid preparation.
TOXICITY/OVERDOSE REACTIONS
Has been defined as “those clinical signs and symptoms that result from an overly high blood level of the drug in various target organs and tissues.†can be absolute or relative.
Predisposing factors:
Patient factors
Age
Weight
Sex (pregnancy)
Diseases – hepatic & renal dysfunction reduced breakdown
Congestive heart failure – less liver perfusion
Genetics – Serum Pseudo cholinesterase deficient
Fearful patients – lower seizure threshold for LA
Drug factors
Vasoactivity – vasodilatation – increase in blood concentration
More concentration – greater risk
Route of Administration – Intravascular – increased toxicity
Rate of injection – slower rate preferred
Vascularity of injection site – more vascular – greater absorption
Presence of Vasoconstrictor – with VC less absorption
Causes of toxicity –
Slow biotransformation
Drug are slowly eliminated by kidney
Too large a total dose
Absorption from injection site is rapid
Accidental intra-vascular injection
Treatment:
• Mild overdose reaction – (agitated, talkative) slow onset reaction – 5-10mins –
PABC that is position the patient comfortably, maintain airway, breathing and circulation.
Administer Oxygen to prevent acidosis, monitor vital signs, in case of convulsions – anti-convulsants (diazepam/midazolam)
• Slower onset – >15 mins – same procedure
• Severe overdose reaction – rapid onset 1 min – (unconsciousness with or without convulsion), patient in supine position, convulsions – protect hand, leg, tongue, BLS, administer anti-convulsant
• post seizure – CNS depression usually present, hence the patient monitored and if the BP drops severly, vasopressors like phenylephrine is given.
IDIOSYNCRASY
Idiosyncrasy is defined may be defined as an individual’s unique hypersensitivity to a particular drug, food, or other substance. It may be genetically determined.
They have no relation to the pharmacology of the drug and may vary in degree from day to day, even in the same patient. e.g. Histamine blockers
The treatment of idiosyncratic reaction depends on the symptoms manifested. The patient’s airway maintained, oxygen administered, circulation evaluated and supported, drugs or parenteral fluids given if required.
ALLERGY
Allergy is an hypersensitive state, acquired through exposure to a particular allergen, re-exposure to which produces a heightened capacity to react.
Predisposing factors
Hyper sensitivity to ester more common (procaine)
Most of patients allergic to methyl paraben, hence it is being widely replaced with Cupryl hydrocuprinotoxin
Allergy to sodium metabisulfite
Latex allergy (cartridge plunger and diaphragm are made of latex)
Signs and symptoms:
Respiratory reactions:
Bronchospasm which constitutes respiratory distress, dyspnea , wheezing ,flushing , cyanosis, perspiration, tachycardia , increased anxiety, use of accessory muscles of respiration.
& Laryngeal edema
Generalized anaphylaxis:
The most dramatic and life-threatening reaction and death can occur in few minutes.
The signs and symptoms are skin reactions, smooth muscle spasm of the GI tract and genito urinary tracts, respiratory distress, cardiovascular collapse.
In rapidly developing reactions all signs and symptoms occur within a very short time.
DENTAL MANAGEMENT IN THE PRESENCE OF ALLEGED LOCAL ANESTHETIC ALLERGY:
Elective dental care – is postponed till definitive allergic test done
Emergency dental care – any one of the following options followed.
Option1: no treatment of invasive nature.
Option2: use general anesthesia
Option3: histamine blockers as local anesthetics
Option4: electronic dental anesthesia or nitrous oxide
MANAGEMENT
Skin Reactions
Delayed – non life threatening reaction – oral histramine blockers- 50 mg diphenhydramine or chlorpheniramine 10 mg – 6th hrly/ 3-4days
Immediate reaction—with conjunctivitis, rhinitis, urticaria- vigorous management.
0.3 mg epinephrine im or sc
50 mg diphenhydramine im
Medical help summoned.
Observe for 60 mins
Oral antihistaminics for 3 days
Respiratory reactions:
Bronchospasm:
Position the conscious patient comfortably.
Definitive care:
1. Terminate treatment
2. Administer oxygen at 5 to 6 liters/min
3. Administer epinephrine 0.3mg im or sc
4. Observe the patient for 60 min. If relapse occurs, re administer
epinephrine 0.3mg
5. Administer histamine blocker 50mg diphenhydramine.
6. Medical consultation
7. Prescribe an oral histamine blocker and complete allergy evaluation
Laryngeal Edema:
Position the unconscious patient in a supine position
1. Epinephrine, administer 0.3mg im or sc every 10 to 15 min if needed. .
2. Maintain the airway
3. Activate emergency medical service
4. Additional drugs: histamine blocker, corticosteroid im or iv
5. Perform cricothyrotomy, if preceding steps have failed to secure a patent airway.