A Quick history on Periodontal Disease
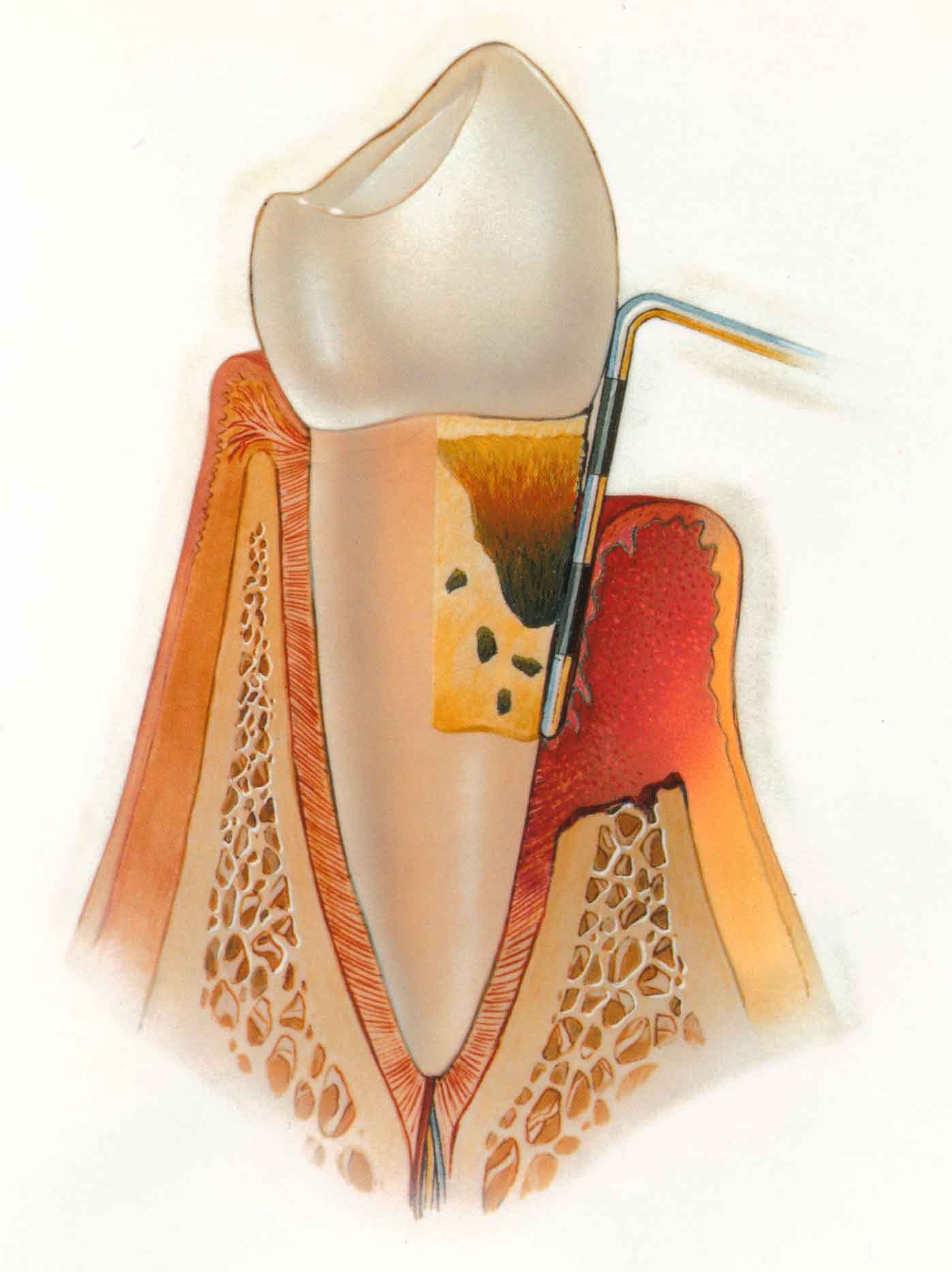
What causes periodontal gum disease ? Our mouths are full of bacteria. These bacteria, along with mucus and other particles, constantly form a sticky, colorless plaque on teeth. Brushing and flossing help get rid of plaque. Plaque that is not removed can harden and form calculus that brushing does not clean. Only a professional cleaning by a dentist or dental hygienist can remove the calculus as it is very hard like pieces of rocks.
The longer plaque and calculus are on teeth, the more harmful they become. The bacteria causes inflammation of the gums leading to gingivitis. In gingivitis, the gums become red, swollen and can bleed easily. Gingivitis is a mild form of gum disease that can usually be reversed with daily brushing and flossing, and regular cleaning by a dentist or dental hygienist. This form of gum disease does not include any loss of jaw bone and tissue that hold teeth in place.
When gingivitis is not treated, it can advance to periodontitis which means that there is inflammation around the tooth as well as jaw bone loss. In periodontitis, the gums pull away from the teeth and form spaces called pockets that eventually become infected. The body’s immune system fights the bacteria as the plaque spreads and grows below the gum line. Bacterial toxins and the body’s natural response to infection start to break down the bone and connective tissue that hold teeth in place. If not treated, the jaw bones, gums, and tissue that support the teeth are destroyed. The teeth may eventually become loose and has to be removed.
Surgical Treatment for Periodontal Disease
- Gingival flap surgery. The basic first line treatment would be to use an ultrasonic scaling to remove the tar tar and calculus. This means the removal of the cause of infection so that finally the healing of the gingival tissue can begin. In most cases, the tooth might have very deep pocketing and subgingival calculus (calculus found on the root of the tooth below the gingival margin) . Sometimes this subgingival calculus can be reached with special types of scalers like a gracey’s currete which goes into the pocket and removes the subgingival calculus. When this special instruments cannot reach the subgingival calculus, a gingival flap or periodontal flap is raised so that there is direct access to the calculus for meticulous removal. After surgery the gums will shrink to fit more tightly around the tooth. This sometimes results in the teeth appearing longer and more fang like.
- Bone and Tissue Grafts. In addition to gingival flap surgery, your periodontist may suggest bone or tissue grafts. Bone Grafting is a way to replace or encourage new growth of jaw bone or gum tissueperiodontitis. A technique that can be used with bone grafting is called guided tissue regeneration, in which a small piece of mesh-like fabric is inserted between the jaw bone and gum tissue. This keeps the gum tissue from growing into the area where the jaw bone should be, allowing the jaw bone destroyed by and connective tissue to regrow.
Different Types of Gingival flap surgery
Apical reposition Gingival flap
In an Apical repositioned gingival flap procedure, a pair of vertical incisions are made at both ends of the neck of the teeth, than a final horizontal incision connecting the two vertical incision is made. The gingiva flap is then peeled back or retracted to expose the jaw bone and roots underneath.
Once exposed, the jaw bone is reshaped. and sometimes augmented with bone-graft material to eliminate bony pockets and to even out the gum margin. After the bone has been re sculpted, the gingiva flap is then replaced back into a position which is closer to the jaw bone line. This results in an even, and well scalloped gum margin. Because of the care taken in reshaping the underlying jaw bone, this gingival flap surgery technique produces much a more aesthetic results than gingivectomy gingiva flap procedure.
Gingivectomy
Gingivectomy is used mostly in the treatment overextended or false gum pocketing. False gum pocketing occurs when there is no bone loss but maybe an overgrowth of the gum tissues instead. This overgrowth allows bacteria to be harbored inside the pocket and cause gingivitis or advanced periodontitis. Therefore the gingiva flap pocket is cut off and the sulcus is reduced to manageable depth, and oral hygiene can resume at normal levels. This type of surgery used to be the gold standard in the treatment of periodontal disease, but patients were left with long teeth and irregular gum margins.