Â
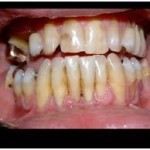
What is Gingival Recession?
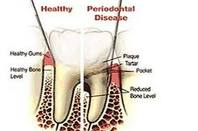
Gingival recession is a dental condition characterized by shrinking gums which expose root surfaces and reduces the zone of attached gingiva. It is a precursor for loss of thin cementum surrounding the teeth and wearing of enamel at the gum line. Exposed root is potentially sensitive via exposed dentinal tubules which can transmit stimuli to the pain receptors in the pulp (inner nerve). Cold, hot and sweet stimuli, drying with an air spray and the use of an ultrasonic scaler results in sensitivity. This situation deters the patient from brushing properly leading to plaque accumulation on the root surface and aggravates the sensitivity. It develops during late teens and early 40’s.
Causes of Gingival Recession
Generalized recession due to gum disease like chronic periodontitis, necrotizing ulcerative gingivitis (trench mouth) and secondary loss from viral diseases such as oral manifestation of HIV. Localized may affect single or multiple teeth and caused by:
- An underlying bony dehiscence with associated tooth-brushing trauma based on its type and technique – vigorous brushing with a stiff or hard toothbrush damaging the gums.
- Excessive and abrasive use of any oral hygiene devices (baking soda and whitening toothpastes) causes cervical abrasion as they strip away the gums and bone supporting the tooth as well as creating notches on the root surface.
- Poor oral hygiene. Those who do not brush and floss enough may cause gum loss through inflammation and infection, even in the absence of gum disease. Bacteria on the plaque release toxic substances that destruct gum tissues.
- Direct gingival trauma from the occlusion such as from a deep overbite depends on how a person brings his teeth together. Excessive forces placed on the tooth brings trauma to the bone and tissues. Excessive pressure from grinding and clenching bends and flexes the teeth. The tooth crystals melt away and the gums lose their attachment. Continuous force leads to bone destruction.
- Frenal pull inserted into an unhealthy gingival margin (thick muscle at the attachment site) interfering with plaque removal and/or pull on the wall of pocket and thereby aggravating the lesion.
- Tooth malposition may predispose to gingival tissue loss as the buccal alveolar plate is thin. Tooth protrudes because of crowding during permanent tooth eruption. There is inadequate jaw bone covering tooth’s root.
- Tooth preparations for restorations such as crown preparations.
- Orthodontic treatment in cases where teeth being larger than size of jaw bone creating prominent roots and causes gums to recede.
- Removable partial denture with a clasp engaging too close to the gums.
10. Post-periodontal or surgical or even non-surgical treatment.
11. Heredity – a person naturally has thin, fragile or insufficient gingival tissue.
Generalized gingival recession tends to be less sensitive than single or multiple sites of localized recession. This is because the root dentine in the former has been irritated by the disease process over a considerable time leading to sclerosis, smear layer, peritubular and secondary dentine formation which acts as a protective layer. The sudden loss of enamel and cementum will trigger an acute sensitivity. Erosion from gastric contents and abfractive lesions contribute to recession.
Management of Gingival Recession
Gingival recession if left untreated leads to lose of dentine and expose roots may become tender, sore, or infected, causing immense pain. It has a greater risk of tooth decay called root caries. The symptoms of gum disease are usually evident before the problem reaches the stage of gum loss, which can be prevented in a patient receiving routine dental care. Diabetics, vitamin C and calcium deficiency patients usually have gum disease. Â A general rule necessitates the use of soft to medium tooth brush which effectively removes plaque. Angulate bristles of the brush along the gum line at a 45 degree angle and apply just enough pressure to slide the bristles below the gum line and brush in a circular motion. Regular flossing and visits to dentist can help prevent gingival recession together with changes in diet. Avoid carbonated and sweetened beverages as they soften the tooth structure making them susceptible to tooth brush abrasion. Toothpaste indicated for sensitive tooth are non-abrasive.
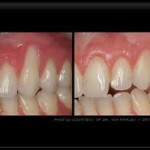
Conservative or surgical management can be done. Dentist performs an examination and takes an X-ray to confirm presence of pockets and level of bone loss. Dentist will roughened the smooth tooth surface with a dental drill and a light coat of adhesive or filling material is applied to the tooth and allowed to set. Surgical management involves gum graft surgery to replace severely damaged tissue. It helps to create more attached gingiva to prevent recession and regenerate and re-establish root coverage. If recession due to periodontal disease, scaling and root planning is done.