What are the causes of ulcers in the mouth?
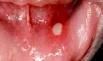
oral ulcer
1. Trauma
i) Mechanical trauma
Accidentally biting your lips or cheeks or brushing your teeth too vigorously to the point of accidentally hitting your gums with the head of your toothbrush can lead to oral ulcers; some people are prone to biting himself because of the presence of a sharp tooth in the mouth.
ii) Chemical trauma
Ulcerations can be caused by irritant or caustic agents such as bleach, concentrated acids, some antiseptic mouthwashes, and even aspirin.
iii) Thermal trauma
Drinking very hot food or drinks can cause ulcers, usually in the palate. It is therefore important, that after dental procedures that requires inferior alveolar nerve anaesthesia (which leaves the entire teeth, gums, tongue, cheeks and lips of the lower jaw on one side unable to sense any pain or heat or taste), a patient should be warned and imformed not to ingest any hot food or drinks, which can lead to ulcerations.
2.Idiopathic/unknown cause, ie. Recurrent aphthous ulcers (RAS)
Recurrent aphthous ulcers are characterized by recurring painful ulcers in the mouth which are round or oval, and have red inflammatory halos surrounding it. Basically oral ulcers that recur and does not seem to be caused by any other known reason, is called RAS, hence RAS is diagnosed by excluding all other reasons of ulceration.
There are 3 types of RAS:
i) Minor RAS– These ulcers are <10mm, ranges from 1-5 in number per episode, and heals in 1-2 weeks without scars. They recur in 1-4 month intervals
ii)Major RAS-These ulcers are >10mm, ranges from 1-10 in number per episode, and heals in >30days with scars. They tend to recur at <monthly intervals, such that in severe cases, the victim experiences new ulcerations before the old one has completely healed, i.e. continuous.
iii)Herpetiform ulcers-Characterized by multiple, small (1-2mm) ulcers which may coalesce to form larger areas of ulceration. As many as a hundred small ulcers can be present at any one point.
3.Infection
i) Bacterial: Tuberculosis (caused by mycobacterias, eg. mycobacterium tuberculosis) can present as ulcers that are painless and covered by a greysih-yellow slough, commonly on the tongue. Syphilis (caused by the spirochaete treponema pallidum) can present as shallow painless ulcers usually on the lips (the primary syphiltic lesion), or as patches of flat ulcerations due to coalescence of multiple ulcers, also known as “snail-track ulcers”(secondary syphilitic lesions)
ii) Viral: Herpes simplex virus (HSV) infection can cause development of numerous small vesicles on any part of the mucosa and lips which eventually ulcerates. The appearance of ulcers usually follow an episode of fever.
4. Systemic diseases
i) Malabsorption in gastrointestinal disorders:
In gastrointestinal disorders like coeliac disease (gluten-sensitive enteropathy) and inflammatory bowel disorders (IBD) like Crohn’s disease and ulcerative colitis, ulcers can also be present in the mouth.
ii) Behçet’s syndrome:
Behcet’s syndrome is a connective tissue disease which may include genital, skin, eyes, or other lesions. The mouth ulcers in Behçet syndrome are often major aphthous ulcers (see RAS above), with frequent episodes and long duration to healing.
iii) Hematinic deficiency (deficiency of blood-forming components):
When there is decreased level of iron, folic acid, or vitamin B12 in the body below the normal range, ulcers can pop up in the mouth. Also, Vitamin B12 is an agent that protects the lining of the mouth, the lack of which breaks down this wall of protection. The decrease in level of hematinics may be caused by lack of consumption, malabsorption, increase in demand, or blood loss. Sometimes hematinic deficiencies are secondary to gastrointestinal diseases as above.
5. Allergies & sensitivities
Allergies or hyperreactivity to preservatives and agents such as benzoic acid (the salts of which are used as preservatives) or cinnamaldehyde (the organic compound found in cinnamon)
6. Immune deficiencies:
Ulcers may be seen in patients whose immune system has been compromised, eg patients with HIV, neutropenias (ulcers appearing on a regular 3-week cycle may indicate cyclic neutropenia) and some other immune defects.
7. Drugs:
Drugs, especially NSAIDs, alendronate (generic name Fosamax; used for treatment of osteoporosis), and nicorandil(vasodilator/potassium channel activator used in angina) may produce lesions in the mouth
8. Stress:
cessation of smoking (for reasons unclear), ulcers appear to exacerbate during school or university examination times.
9. Hereditary
RAS is sometimes inherited. Hence a patient presenting with recurring ulcers from childhood not associated with any other causes listed here, and has a parent or sibling with RAS, is almost certainly suffering from the same condition.
10. Malignancy
If an ulcer does not heal, one should suspect malignancy and further tests should be done to confirm it.
11. Endocrine/hormonal factors
This is related to the progesterone level changes during menstruation and pregnancy. However, not all women get mouth ulcers associated with hormonal level changes.

