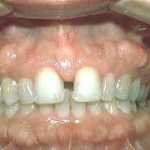
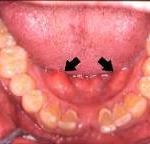
Intra-oral bony growths of all types, present a clinical challenge for the dental team attempting to capture accurate detail for final impressions of crown and bridge, removable prosthetics, oral appliances, accurate opposing models, study models, and whitening trays. Stock impression trays often can’t be seated to depth, because they get hung up on these bony anatomical variants, or the bony protuberances can cause pain during the impressioning procedure, as there is often only a thin membrane of covering tissue which is easily irritated. Lingual tori may also limit the space for the tongue and can result in speech impediment. Even though these bony areas can create a clinical challenge with impressioning, these areas are prime sites for harvesting autogenous bone for bone grafting of dental implants and can be used for multiple reconstructive procedures such as nasal reconstruction.
Bony exostosis is described as a benign localized overgrowth of bone of unknown or controversial etiology, however the hypothesis is that there may be an interplay of genetic and environmental factors including severe occlusal stress. Buccal bony exostoses have been reported secondary to soft tissue graft procedures and free gingival grafts with periosteal trauma seemingly the main etiologic agent. In a study of 960 Thias, Jainkittivong found that 26.9% of the sample exhibited exostoses, which were more prevalent in the male maxilla, and most of the exostoses were located on the buccal of the jaws. In a study by Horning buccal alveolar bone enlargements were found in 25% of all teeth examined; 18% were expressed as marginal bony lippings and 7% as buccal exostoses. Small exostoses called palatal tubercles were present in 56% of all skulls examined by Sonnier which can require their removal for adequate flap adaptation after surgical procedures. However, it is the presence of buccal exostoses that may require impression tray modification when they interfere with the path, insertion and final position of the tray.
The torus has been mentioned in the literature for about 180 years and has been described as a benign, anatomical, slowly growing bony prominence occurring in the hard palate and the lingual aspect of the mandible or an area of hyperostosis. Although the etiology of Torus Palatinus and Torus Mandibularis is debated, tori seem to be a functional reaction to masticatory stresses and are due to genetic and environmental factors with suggestions of autosomal dominant transmission. The reported literature on the occurrence of tori in the population varies with different ethnicity and sex. In most studies, ranges from 1.4 – 69.7 percent are reported, while one publication states that tori occur 100% amongst Greenland Eskimos. In some ethnic groups women are more likely to have larger torus palatinus, whereas men have larger torus mandibularis and there seems to be a strong link between the coexistence of palatal and mandibular tori. There may also be a positive relation for postmenopausal Caucasian women between the bone mineral density and torus size. In a study of 400 Japanese the reported risk factors for mandibular lingual torus were gender, number of sound teeth and bruxism, and for palatal torus the risk factors were gender and TMJ symptoms. The number of remaining sound teeth also showed a positive correlation to tori prevalence in a Norwegian study. The prevalence of torus mandibularis and parafunctional activity is higher in temporomandibular disorder than controls. There seems to be a correlation between the presence of mandibular tori and the ability to maintain favourable bone height, with a suggestion that a genetic locus for this may shed some light on the genetic contribution and mechanisms that tend to make the marginal alveolar bone more resistant to destructive agents.
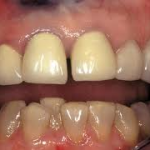
Malpositioned lower front tooth
Teeth that are mal-positioned in the dental arch often create a path of insertion problem when attempting to take final impressions. Often the maxillary canine is crowded and labially displaced. On the mandibular arch, the lower anteriors are often crowded, displaced, or rotated with lower first and second premolars often lingually displaced, making it impossible to seat a traditional impression tray. The creation of traditional custom impression trays for these clinical situations is often frustrating, time consuming, costly and the clinician wastes valuable operatory time. The availability of an instant “custom tray” allows for immediate treatment and impressioning.
The presence of tori can complicate fixed prosthetic reconstruction, the fabrication of dentures, and any other oral appliance such as bruxism splints, mouth guards, and orthodontic appliances, with the clinical process of taking an accurate impression one of the most difficult tasks the clinician faces. Maxillary stock trays will often not seat deep enough in the buccal vestibule when there is a large torus palatinus, complicating the capture of detail, with resultant lack of control of the impression material towards the soft palate and throat, and loss of directional drive of the impression material which is critical in final crown and bridge impressions.