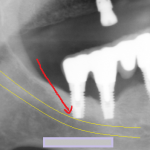
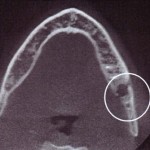
- for determining the location of the inferior alveolar nerve in all three dimensions of the mandible (lower jaw). With the software that is available to the dentist, the radiographic information from this study can be used to manipulate the jaw in 360° and provide the most accurate information to the dentist for treatment planning for the placement of the implant or for a third molar extraction. When screening radiographs demonstrate the increased risks for implant placement or third molar extraction, it is below the standard of care for the dentist or oral surgeon to fail to explain the
advantages of the CT or CBCT as a diagnostic option to the patient before the patient is subjected to the increased risk of nerve injury.
-
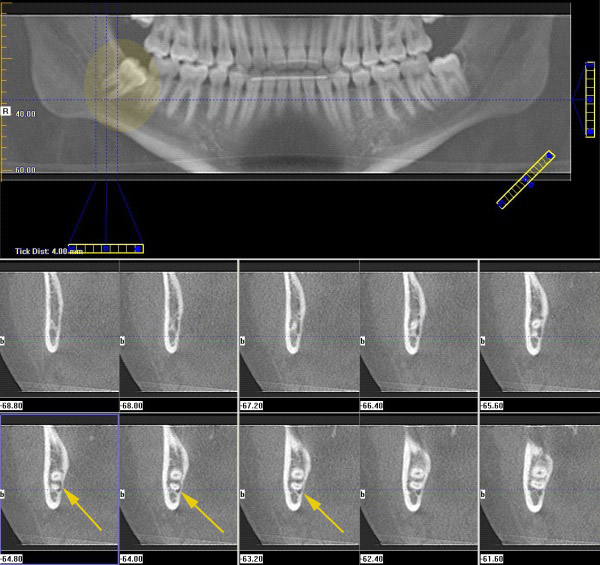
When the dentist has inadequate information or reads the panorex x-ray or the periapical x-ray incorrectly, he/she is at greater risk of injuring the inferior alveolar nerve while drilling the hole to place the implant in. Unfortunately, there are occasions when the inferior alveolar nerve itself can branch, leaving one canal with calcified borders, and 1-2 other branches that may or may not have radiographically evident borders. This anatomical variation may be missed in periapical and panorex imaging, and may not always be identified in Cone Beam C.T. imaging either.
No dentist takes an x-ray with the dental drill in place, but frequently there is an x-ray with the implant seen violating the mandibular canal or touching it. Since the x-ray is in two dimensions, one cannot say the implant is in the canal, verses just overlapping the canal on the tongue (lingual) side or on the cheek (buccal) side of the canal. It is suspected that the drill preparation can violate the mandibular canal with poor technique, even though the post-operative radiograph of the implant in place shows the implant to be the appropriate 2mm above the canal. If the patient has anesthesia/paresthesia/dysesthesia symptoms, the dentist should know that he/she may have injured the inferior alveolar nerve with the drill when placing
the implant or the implant is in the canal or impinging on the canal putting pressure on the inferior alveolar nerve.
The standard of care requires the dentist to promptly remove the implant if the patient has immediate symptoms that reflect a compromise of the inferior alveolar nerve. Sometimes the implant can compress the bone below the tip of the implant, putting pressure on the inferior alveolar nerve. The pressure on the inferior alveolar nerve can cause symptoms of numbness, tingling etc. and when the implant is backed out the nerve may return to normal over time.
It is negligent for a dentist not to remove an implant when it is causing immediate nerve symptoms. If the implant is causing symptoms, the dentist should take an x-ray to evaluate the implant and simply remove the implant. A Cone Beam CT scan (CBCT) can demonstrate that the dentist did indeed place the implant into the mandibular canal by showing where the missing bone is or the different density of the bone that has filled in. If there is a delay in the removal of the problem implant after there has been full osseous integration around the implant (the living bone has grown around the threads of the implant), later removal can be problematic because now the implant can’t be backed out and needs surgical removal with the inherent risk of additional nerve injury.
2) Negligent Root Canal Treatment
3) Negligent Fracture of the Mandible
It is negligent for a dentist to exert so much force during the extraction of a lower tooth as to cause a fracture of the mandible that cause injury to the inferior alveolar nerve. Sometimes a tooth is fused or ankylosed to the surrounding bone and it will not
budge when the dentist tries to elevate it out using routine technique. More force is not called for in this situation. The tooth should be accessed and sectioned into pieces so as to avoid injury to surrounding anatomy. When a dentist uses brute force and ignorance, he/she can cause a fracture of the lingual plate causing injury to the lingual nerve and with extreme force the
mandible can be fractured clean through causing a violation of the mandibular canal and injuring the inferior alveolar nerve.
A pre-operative panoramic radiograph may warn of a thinned and fragile mandible and provide the dentist with additional information regarding the risks of fracture that may require the skills of an oral maxillofacial surgeon. At a minimum, the dentist is required to inform the patient of this additional risk and give the patient the option of having the tooth extracted by an oral maxillofacial surgeon. Under these circumstances, the general dentist is well advised to insist on referring the patient to an oral maxillofacial surgeon for the extraction of this lower molar.
4) Local Anesthetic
 Generally speaking, it is not below the standard of care for the dentist to injure the inferior alveolar nerve in the delivery of local anesthetic for a mandibular block. The mandibular block is a procedure of giving anesthesia to the mandibular region to block certain areas from experiencing pain when the dentist needs to perform dental surgery in the oral cavity. However, if the needle actually hits the nerve, making the patient jump, or if blood shows during aspiration (the dentist is required to pull back on the syringe plunger to make sure he/she is not in an artery) before injecting the local anesthetic, the needle should have been backed off slightly before injecting the anesthetic. A needle strike of the nerve can be masked if multiple injections are needed to achieve anesthesia.
Generally speaking, it is not below the standard of care for the dentist to injure the inferior alveolar nerve in the delivery of local anesthetic for a mandibular block. The mandibular block is a procedure of giving anesthesia to the mandibular region to block certain areas from experiencing pain when the dentist needs to perform dental surgery in the oral cavity. However, if the needle actually hits the nerve, making the patient jump, or if blood shows during aspiration (the dentist is required to pull back on the syringe plunger to make sure he/she is not in an artery) before injecting the local anesthetic, the needle should have been backed off slightly before injecting the anesthetic. A needle strike of the nerve can be masked if multiple injections are needed to achieve anesthesia.
If the Inferior alveolar nerve is blocked with the anesthesia solution, then the whole nerve along with its subdivisions, including the mental nerve, incisive nerve, lingual and the long buccal nerve are blocked for a limited period of time from transmitting pain stimuli to the brain. The basic idea is to use anatomical landmarks to place the tip of the syringe in the approximate area where the inferior alveolar nerve enters the mandibular canal. Due to the differences in every person’s anatomy, the dentist cannot guarantee that the needle will not actually hit the inferior alveolar nerve, causing a partial nerve injury with paresthesia/dystesthesia.
These injuries usually resolve, but on rare occasions can develop into a sustained neuropathic pain. The dentist does have an obligation to chart your nerve injury and to map it in the chart, so as to follow it accurately for healing. If the symptoms are improving with respect to intensity and distribution, the dentist may not need to refer the patient to an oro-facial pain specialist.
If there is significant paresthesia/dysesthesia and it is not resolving, the patient should be referred to an oral surgeon who specializes in microsurgery and/or an oro-facial pain specialist before the fourth month of the injury. Most neurologists do not specialize in these injuries and you are better off being seen by the oral surgeon/oro-facial pain specialist before the pain
becomes centralized to the brain and your treatment options become seriously diminished. The longer you wait, the less likely surgery will be an option for you.