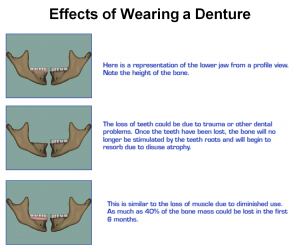
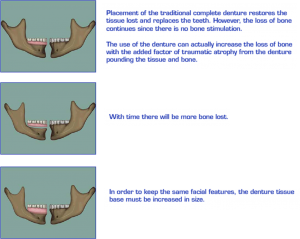
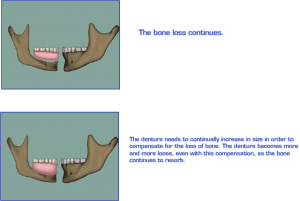
Introduction
Alveolar ridge resorption or deficiency occurs in a variety of forms which is undercuts knife edge appearance, concave ridge form rather than convex and severe resorption patterns such as the very flat pencil thin mandible.
The ability of the patient to wear a conventional denture satisfactorily depends on
A proper convex ridge form
Adequate alveolar ridge height
Adequate surface area of a non mobile keratinized mucosal base.
The degree of resorption is dependent on a variety of local and systemic factors such as
Systemic bone disease
Poor nutrition
Size and shape of the alveolus and effect of ill fitting dentures
Similarities in resorption patterns of maxillary and mandibular ridges. J Prosthet Dent. 1978 Jun;39(6):598-602
The mandible does not progressively widen as its opposing maxillae becomes narrower, nor does a progressive incremental increase occur in posterior maxillomandibular width relations with increased resorption or resorptive age.
The arch width of the mandible exceeds the arch width of the maxillae in the molar region by an average of 6 to 7 mm after sufficient resorption established a definitive alveolar crest.
The progressive and irreversible mandibular alveolar resorption rate is greatest in the earlier stages of edentulism and slows with loss of bone, longevity of edentulism, and attendant wearing of dentures.
Functional effects of edentulism
The maxillomandibular relationship is altered in all spatial dimensions.
Progression toward decreased overall lower facial height, leading to the typical overclosed appearance.
Progressive instability of conventional soft tissue – borne prosthetic devices.
Neurosensory changes secondary to atrophy, and in all three dimensions.
Systemic factors.
Resorptive pattern of the edentulous ridge (Mercier, 1995)
The ridge is wide enough at its crest to accommodate the recently extracted teeth. Type I – Minor ridge modelling.
The ridge becomes thin and pointed. Type II – Sharp atrophic residual ridge
The pointed ridge flattens to the level of the basal bone. Type III – basal bone ridge
The flattened ridge becomes concave as the basal bone resorbs. Type IV – basal bone resorption
Maxilla
Resorption of the maxilla is on the buccal and inferior portion of the alveolar ridge resulting in upward and inward loss of bone.
In anterior maxilla there is less horizontal bone loss and posterior drift of the anterior crest.
In the posterior maxilla there is inward drift of posterior crest.
Mandible
The mandible resorbs downwards and outwards.
Rapid flattening of the alveolar ridge is seen
Objectives of ridge reconstruction:
To eliminate preexistent or recurrent pathology.
To rehabilitate infected or inflamed tissue.
To reestablished maxillomandibular relationships in all spatial dimensions.
To preserve or restore alveolar ridge dimensions (height, width, shape, and consistency) conducive to prosthetic restoration.
To achieve keratinized tissue coverage over all load bearing areas.
To relieve bony and soft tissue undercuts.
To establish proper vestibular depth and repositioning of attachments to allow for prosthetic flange extension if necessary.
To establish proper notching of the posterior maxilla and palatal vault proportions.
To prevent or manage pathologic fracture of the atrophic mandible.
To prepare the alveolar ridge by onlay grafting, corticocancellous augmentation, sinus lift, or distraction osteogenesis for subsequent implant placement.
To satisfy facial esthetics, speech requirements, and masticatory challenges.
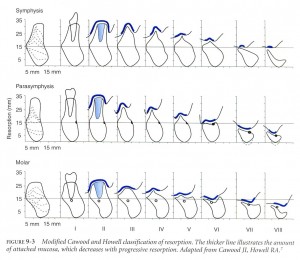
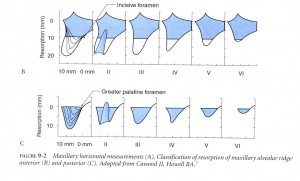
Residual ridge form has been classified by Cawood and Howell as follows:
Class I – dentate
Class II – post-extraction
Class III – convex ridge form, with adequate height and width of alveolar process.
Class IV – knife edge form with adequate height but inadequate width of alveolar process.
Class V – flat ridge form with loss of alveolar process.
Class VI – loss of basal bone that may be extensive but follows no predictable pattern.
Indications for Ridge Augmentation
Progressive loss of denture stability and retention.
Loss of alveolar ridge height, width and decreased vestibular depth and denture bearing area.
Considerable basal bone resorption in the mandible, resulting in neurosensory disturbances
Increased susceptibility to fracture of the atrophic jaws.
Replacement of necessary supportive bone.
Altered interarch relationship
Maxillary Procedures
Maxillary augmentation:
Onlay bone grafting – Autogenous / allogenic grafts.
Alloplastic onlay grafting.
Interpositional / sandwich grafts.
Sinus lift procedure.
Mandibular augmentation:
Superior border augmentation.
Iliac crest, rib graft, hydroxyapatite
Inferior border augmentation
Autogenous or allogenic freeze dried cadaveric mandible.
Interpositional / sandwich bone grafts
Visor osteotomy
Onlay grafting
Autogenous, allograft and alloplastic.
Ridge split osteoplasty
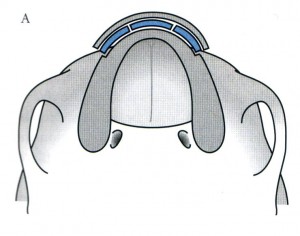
Bone cuts and the position of the fragment after the osteotomy. The defect is filled with interpositional graft (blue) to maintain increased buccolingual width.
Mandibular Procedures
The goals of surgical treatment to augment the mandible include:
Providing optimum ridge form for the support of a prosthesis.
Improvement of the maxillomandibular relationships.
Increasing the bony bulk of the mandible.
Providing adequate bone for implant placement in selected patients.