Continued from Part 1
Incorporation of pigments into the dental hard tissues during their formation
This occurs in congenital disorders associated with hyperbilirubinemia, congenital porphyria and tetracycline pigmentation.
Congenital hyperbilirubinemia (neonatal jaundice)
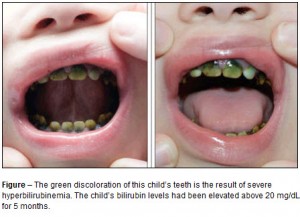
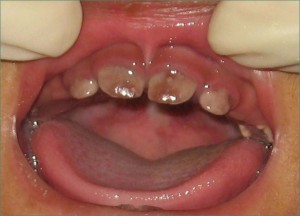
Mild transient jaundice (yellowing of the skin and the whites of the eyes caused by an accumulation of bile pigment (bilirubin) in the blood) is common in newborns but in severe cases, most frequently associated with hemolytic disease of the newborn (rhesus incompatibility), bile pigments may be deposited in the calcifying enamel and dentine of developing teeth, particularly along the neonatal incremental line. The pigment is largely confined to the dentine, the affected teeth being discolored green to yellowish-brown. Enamel hypoplasia may also occur.
Congenital porphyria
This is a rare, recessive autosomal disease in which there is an inborn error of porphyrin metabolism. It is characterized by the excretion of red porphyrin pigments in the urine and circulating porphyrins in the blood which are deposited in many tissues, including bone and dental hard tissues. Affected teeth show a pinkish-brown discoloration and a red fluorescence under ultraviolet light.
Tetracycline pigmentation
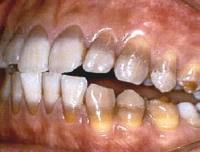
Systemic administration of tetracyclines during the period of tooth development results in their deposition in the dental hard tissues as well as in bone. Dentine is more heavily stained than enamel and in ground sections of affected teeth yellow bands of pigmentation related to incremental lines in dentine can be seen. The pigmented bands fluoresce a bright yellow under ultraviolet light. Tetracyclines are also deposited in cementum.
Affected teeth generally are yellowish when they erupt and become darker and browner after exposure to light. The degree of clinical discoloration of the teeth is affected by which particular tetracycline preparation has been taken, the dosage and the age of the patient at the time of administration of the drug. If the drug is administered when crown formation is already complete, then the tetracycline is confined to the roots and the discoloration on teeth will not be clinically discernible.
Tetracyclines cross the placenta and baby teeth discoloration may occur if the drug is given any time from 29 weeks to full term. It is particularly important to avoid tetracyclines from 4 months to about 7 years of age if severe clinical discoloration of the permanent dentition is to be prevented.
Possible treatment options for discolored teeth
Prophylaxis paste
Simple extrinsic stains can be removed with a mixture of pumice powder and toothpaste or an abrasive prophylaxis paste together with a bristle brush should remove the stain. Proper oral hygiene procedures should be practiced to prevent recurrence.
Acid pumice abrasion technique or microabrasion
This technique is used only for surface enamel defects. There are two approaches:
Hydrochloric acid technique (quicker)
A mixture of 18% hydrochloric acid and pumice is applied to the affected area using a wooden stick. The mixture is rubbed into the surface for 5 seconds and then rinsed away. These two steps are repeated (maximum of 10 times – removing <0.1mm enamel) until the desired color change is achieved. The enamel is then polished and a fluoride solution applied.
Phosphoric acid technique (slower but potentially safer)
A number of variations of this technique is used. A commonly used method is to etch with 30-50% orthophosphoric acid for 1 – 2 minutes, wash, then pumice slurry on rubber prophy cup for 1 minute wash. Repeat etch and pumice stage twice more., washing between. Dry tooth and apply topical fluoride solution. May be repeated up to twice more, but least at least 6 weeks before each repeat to check for improvement.
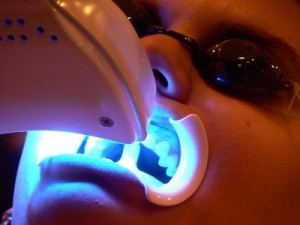
Vital bleaching agents using carbamide (or urea) peroxide
Advantages
- Work best with extrinsic stains and quite well for many intrinsic stains.
- Easily applied in custom trays, nondestructive and easily repeated if necessary.
- Does not alter the underlying tooth shade or translucency. If sufficient and even lightening of the shade is achieved, bleaching produces the best appearance of all options.
- Can also be used to mask severe staining before a veneer is placed. This prevents the dark enamel showing through and allows a more translucent veneer to be used, improving the final appearance.
Disadvantages
- Unpredictable effectiveness with tetracycline teeth discoloration, often leaving a dark zone cervically where the stained root shows through the thin cervical enamel. However almost always some improvement and this may satisfy the patient.
- Only appropriate when there are minimal or no restorations in the teeth. Restorations are not bleached and there is a theoretical concern that bleaching agents might track to the pulp along the margins of restorations.
- Some over-the-counter formulations are acidic and others may cause local soft tissue irritation, and should not be encouraged.
Non-vital bleach
Advantages
Allows bleaching of deeper dentine than vital bleach, producing greater effect.
Disadvantages
- Only possible in non-vital teeth and so usually inappropriate for multiple teeth.
- To bleach dentine below the cervical enamel the bleaching agent must be applied to the cervical part of the root canal as well as the pulp chamber.
Direct composite, indirect composite or porcelain veneers
Advantages
Good appearance possible, can be as good as crowns but much less destructive.
Disadvantages
- Some tooth preparation is required, the amount varying slightly between types.
- When placed over darkly stained teeth, veneer and cement must be opaque. This reduces translucency and produces a ‘flat’ artificial color to finished restoration.
Crown
Advantages
- Strong and retentive
- Very darkly stained teeth are best crowned
- The porcelain is thicker than veneer so that opaque materials are not required. If necessary, metal-bonded crowns completely mask the underlying color.
- Usually the best alternative if the discolored tooth contain extensive restorations
- Appearance can be excellent
Disadvanges
- Destruction of tooth tissue
- Margins may compromise gum health
- Expensive