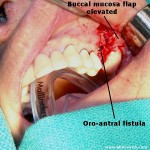
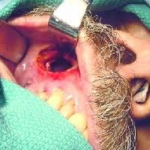
This is a fistulous communication between the floor of the maxillary sinus to the oral cavity. This commonly occurs following dental extraction of infected upper molar and premolar tooth. From a small cavity at birth, the maxillary sinus starts to enlarge during the third month of foetal life and usually reaches maximum development around the eighteenth year. Its volume is approximately 20-25 ml in a normal adult. The floor of the sinus consists of the alveolar process and the hard palate.
The upper lateral teeth when removed have a tendency to form blood clots. Fibrosis sets in within the clot material aiding the healing process. Fibrosis inside the clot is the most critical stage in the healing process. During this process of healing the air pocket within the maxillary sinus could keep constantly extruding hampering the healing process. This eventually leads to the formation of oroantral fistula. In order to prevent this fistula formation the mucosal flaps after extraction of upper lateral teeth should be sutured.
Clinical features:
1. Patients manifest with signs and symptoms of maxillary sinus infections.
2. Purulent discharge could be seen from the middle meatus
3. History of dental extraction – positive
4. Fistulous communication could be seen within the oral cavity through which pus could be seen extruding
Valsalvin test: This is confirmatory test for the presence of oroantral fistula. This test is performed by asking the patient to blow air through the nose after pinching the nose closed. The patient must keep the mouth open. The air could be heard hissing out of the fistula. This test could be negative in some patients in whom oedematous middle ear mucosa occludes the fistula (false negative).
Probe test: using a blunt probe, an attempt should be made to probe the suspected fistulous area.
Radiology:
 1. X ray para nasal sinuses water’s view shows haziness of the involved maxillary antra.
1. X ray para nasal sinuses water’s view shows haziness of the involved maxillary antra.
2. CT scan of para nasal sinuses is diagnostic. The defect can be clearly seen ion the bone window cuts.
Management:
1. Wait and watch approach: A significant amount of these fistulas tend to heal spontaneously. This is more so if the size of the fistula is 2 mm or less. If the size is 3 mm or more then spontaneous healing is hampered because of sinus infection in the periodontal area.
2. Caldwel Luc procedure: This surgery aims at creating a more permanent drainage via the antrostomy performed through the inferior meatus. This helps in spontaneous healing of the fistula.
3. Direct closure of the fistula can be attempted using palatal flaps. The aim was to provide support for the blood clot in the socket so that it will organize, be replaced by bone and epithelialize on its oral and antral surfaces.
The clot in the cavity should be protected with a gauze sponge dressing for 48 h. A figure-of-eight wire or an acrylic splint may also be applied for additional support to healing of the tissues. Furthermore, the patient should be motivated to avoid intraoral negative pressure such as blowing the nose and to use antibiotics for prophylaxis.
A palatal flap (PF) was preferred in the cases who had reduced depth of the buccal sulcus due to an unsuccessful previous attempt at closure of an OAF.
4. Sliding bridge flap. A sliding bridge flap (SBF) was used in cases which were totally edentulous and had a reduced sulcus depth due to alveolar resorption. Mucoperiostium overlying an edentulous ridge in the vicinity of the fistula has been utilized in the form of a SBF. Buccal vestibular sulcus height was not affected in those cases.
The preferred technique may vary from one clinic to another, depending upon past experience. In addition to the above mentioned techniques, the use of some alloplastic materials has also been proposed. Materials ranged from autogenous bone grafts to gold foil. With advancing technology, dura mater and fascia lata, as examples of allotransplants, have also been used for closing OAF. In recent years, the Use of a pedicled buccal fat pad in closure of large oroantral openings has become popular. Attempts to close larger defects caused by severe trauma or tumours by local flaps may lead to failure. Distant flaps from the extremities or forehead or tongue flaps have been described earlier. Successful closure of OAF is dependent on the absence of pathology within the sinus and a proper surgical technique.
High incidence of chronic sinusitis or antral polyps may be the most commonly associated cause of OAF formation. Otherwise, in a case with a healthy sinus wall and mucosa, the opening of the sinus will repair spontaneously following injury caused by tooth extraction. Also the length and width of the extraction socket is of importance. Shorter and wider extraction sockets are unfavourable to spontaneous closure.