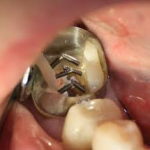
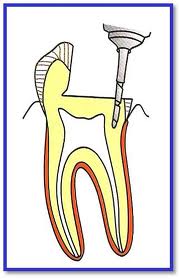
When the teeth are decayed and it has to be restored the dentist goes for the filling but sometimes the decay is extensive and a large part of the tooth is lost. In such cases pins and posts are used as the simple filling material can not give the adequate strength to sustain the masticatory forces and fractures. The pins and posts can be used separately or together as decided by the dentist.
Pins in Dentistry
There are many types of pins available in dentistry. They are basically thin metallic shafts. They are either cemented in the tooth after making the space for them or they are screwed in the tooth. They are used to give the strength to the filling. First the pins are placed in the tooth above that core built up is done and after that crown is given above that.
INDICATIONS
- As additional aids of retention in badly broken down or mutilated teeth.
- In teeth with poor prognosis i.e. endodontically and periodontically involved teeth.
- When one or more cusps need capping.
- Increased resistance and retention form is needed.
CLASSIFICATION
1. Direct/non parallel pins- are inserted into Dentin followed by placement of restorative material directly over them.
Three major categories of direct pins are:
Cemented pins- pins are 0.001-0.002 inch smaller than their pin channels and the difference in diameter provides space for cementing medium. Are least retentive but virtually place no stress on surrounding dentin during or after placement.
Friction locked pins- are 0.001 inches larger than their pin channels and hence utilize the elasticity of dentin for retaining the tapped pins in a vise like grip. Better retention than cemented pins but generates stresses in dentin in the form of cracks or craze lines.
Threaded pins- are 0.0015-0.002 inches larger than their pin channels and like friction locked pins they are also retained by elasticity of dentin. Provides maximum retention but at the same time generates excessive stresses in the form of cracks in dentin.
Four sizes of TMS pins.
• Regular ( 0.031 inch [0.78 mm]
• Minim (0.024 inch [0.61 mm]
• Minikin (0.019 inch [0.48 mm]
• Minuta ( 0.015 inch [0.38 mm]
2. Indirect/parallel pins- are an integral part of Cast restoration. These pins are placed parallel to each other as well as parallel to the path of insertion of the restoration.
MATERIALS USED
1. Stainless steel
2. Titanium
3. Silver
4. Cast gold alloys
5. Platinum-palladium
6. Platinum-iridium
7. Plastic
8. Aluminium
9. Acrylic
PRINCIPLES OF PIN PLACEMENT
Most desirable locations for pin holes are corners of the tooth and least desirable are in the middle of facial, lingual, mesial and distal surfaces of a tooth.
Dentist should try and place pins in locations where they will be surrounded by optimum bulk of dentin and restorative material.
Pin-retained Silver Amalgam
« If a base is needed within the prep, it should be placed BEFORE the pin is placed so as not to engulf the pin in base.
« Base should stay away from the Dentino-enamel junction, especially where the pin will be placed.
« Pins are not placed into bases.
Posterior Pin Selection
« The TMS pins of choice for posterior broken down teeth are the MINIM (.024 inch) and the MINIKIN (.019 inch).
«  The MINUTA (.015 inch) is usually too small for posterior teeth, however the REGULAR (.031 inch) should not be used because of the great stress and crazing that can be created.
FACTORS AFFECTING PINS
1. Pin Orientation Â
2. Number of Pins Â
3. Diameter of Pins
1. Pin Orientation
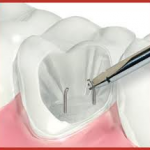 With multiple pins, orientation to one another in a non-parallel way will increase retention of the restoration.
With multiple pins, orientation to one another in a non-parallel way will increase retention of the restoration.
2. Numbers of Pins
- Within reason, increasing the number of pins increases the retentiveness of the restoration.
- With more pins:
- risk of crazing increases    Â
- available dentin decreases
- strength of the restoration decreases
3. Diameter of Pin
- Within reason, as the diameter of the pin increases, so does retention in dentin and of the restoration.
Orientation – Number – Diameter of Pins
- As Number, Diameter, and Depth of pins in the tooth increases so does retention of both pins and restorations.
- However, so also increases the chance for Pulpal Penetration or External Tooth Perforation.
- Â For self-threading pins, NO increase in retention is gained beyond embedment of 2mm.
ADVANTAGES
- Offer retention without the need for extensive preparation of tooth structure.
- May increase resistance form of the tooth preparation to some extent.
- Less time consuming and less expensive than cast restorations which require multiple appointments.
DISADVANTAGES
- Do not increase the strength of the overlying restorative material.
- Induce stresses in dentin in the form of cracks or craze lines, which may increase the potential for the fracture of tooth, micro leakage, pulpal damage etc.
- Increase the chances of perforation into pulp or on the external tooth surface.