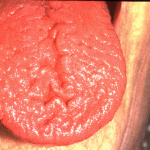
Burning mouth syndrome (BMS) is a painful, frustrating condition often described as a scalding sensation in the tongue, lips, palate, or throughout the mouth. Although BMS can affect anyone, it occurs most commonly in middle-aged or older women.
BMS often occurs with a range of medical and dental conditions, from nutritional deficiencies and menopause to dry mouth and allergies. But their connection is unclear, and the exact cause of burning mouth syndrome cannot always be identified with certainty.
Other names for burning mouth syndrome include scalded mouth syndrome, burning tongue syndrome, burning lips syndrome,
glossodynia and stomatodynia.
Signs and Symptoms
Moderate to severe burning in the mouth is the main symptom of BMS and can persist for months or years. The pain from burning mouth syndrome typically has several different patterns. It may occur every day, with little pain when you wake but becoming worse as the day progresses. Or it may start as soon as you wake up and last all day. Or pain may come and go, and you may even have some entirely pain-free days. For many people, the burning sensation begins in late morning, builds to a peak by evening, and often subsides at night. Some feel constant pain; for others, pain comes and goes. Anxiety and depression are common in people with burning mouth syndrome and may result from their chronic pain.
Other symptoms of BMS include:
- tingling or numbness on the tip of the tongue or in the mouth
- bitter or metallic changes in taste
- dry or sore mouth.
Burning mouth syndrome usually does not cause any noticeable physical changes to your tongue or mouth.
Causes
There are a number of possible causes of burning mouth syndrome, including:
- damage to nerves that control pain and taste
- hormonal changes
- dry mouth, which can be caused by many medicines and disorders such as Sjögren’s syndrome or diabetes
- nutritional deficiencies
- oral candidiasis, a fungal infection in the mouth
- acid reflux
- poorly-fitting dentures or allergies to denture materials
- anxiety and depression.
The cause of burning mouth syndrome can be classified as either primary or secondary.
Primary burning mouth syndrome
When the cause of burning mouth syndrome isn’t known, the condition is called primary or idiopathic burning mouth syndrome. Some research suggests that primary burning mouth syndrome is related to problems with taste and sensory nerves of the peripheral or central nervous system.
Secondary burning mouth syndrome
Sometimes burning mouth syndrome is caused by an underlying medical condition, such as a nutritional deficiency. In these cases, it’s called secondary burning mouth syndrome.
In some people, burning mouth syndrome may have more than one cause. But for many, the exact cause of their symptoms cannot be found.
Risk factor
Burning mouth syndrome usually begins spontaneously, with no known triggering factor. But some research studies suggest that certain factors may increase your risk of developing burning mouth syndrome. These risk factors may include:
- Being a so-called “supertaster,” or someone with a high density of the small tongue bumps called papillae, which contain taste buds
- Upper respiratory tract infection
- Previous dental procedures
- Allergic reactions to food
- Medications
- Traumatic life events
- Stress
Diagnosis
A review of your medical history, a thorough oral examination, and a general medical examination may help identify the source of your burning mouth. Tests may include:
- blood work to look for infection, nutritional deficiencies, and disorders associated with BMS such as diabetes or thyroid problems
- oral swab to check for oral candidiasis
- allergy testing for denture materials, certain foods, or other substances that may be causing your symptoms.
Treatment
Treatment should be tailored to your individual needs. Depending on the cause of your BMS symptoms, possible treatments may include:
- adjusting or replacing irritating dentures
- treating existing disorders such as diabetes, Sjögren’s syndrome, or a thyroid problem to improve
burning mouth symptoms - recommending supplements for nutritional deficiencies
- switching medicine, where possible, if a drug you are taking is causing your burning mouth
- prescribing medications to
- relieve dry mouth
- treat oral candidiasis
- help control pain from nerve damage
- relieve anxiety and depression.
When no underlying cause can be found, treatment is aimed at the symptoms to try to reduce the pain associated with burning mouth syndrome.
Helpful Tips
You can also try these self-care tips to help ease the pain of burning mouth syndrome.
- Sip water frequently.
- Suck on ice chips.
- Avoid irritating substances like hot, spicy foods; mouthwashes that contain alcohol; and products high in acid, like citrus fruits and juices.
- Chew sugarless gum.
- Brush your teeth/dentures with baking soda and water.
- Avoid alcohol and tobacco products.
Talk with your dentist and doctor about other possible steps you can take to minimize the problems associated with burning
mouth syndrome.