What is Bulimia Nervosa?
Bulimia, also called bulimia nervosa, is an eating disorder that involves binging and purging. Binge-eating is when a person eats an abnormally huge amount of food in a short period of time. The food is usually consumed not in response to hunger, but to depression, stress or self-esteem issues. In fact, a person may experience loss of control and continue binging even on a full stomach. This is then followed by purging, which are efforts to lose weight such as self-induced vomiting, long hours of excessive exercise, taking laxatives and diuretics. The most common method is self-induced vomiting, which is done by sticking a finger down the throat following an episode of over-eating so that food is vomited out before it is absorbed by the body.
What are the signs of a bulimic person?
It is hard to identify a bulimic person because unlike people with aneroxia, bulimics appear normal, and can even be overweight. Furthermore, they tend to perform their acts of binging and purging behind closed doors, like hiding food in their drawers, or going into the kitchen after everyone has slept.
What are the harmful effects of bulimia to the teeth?
A bulimic can hide behind closets and toilets all they want, but they can’t hide the effects that purging (self-induced vomiting) has on their mouth and teeth. Here are some of them:
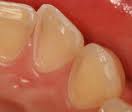
- Dental erosion: As food is swallowed, gastric acids are produced to break down the food particles. When food is vomited out of the body intentionally, these acids are also expelled from the mouth. In the process, they come in contact with the teeth, particularly the surfaces facing the inside of the mouth (the lingual surfaces) of the upper front teeth. Over a period of time, these acids can cause tooth enamel to erode, exposing the dentine and even pulp. This can cause sensitivity of teeth.
- Following vomiting, the bulimic may brush her teeth to eliminate the taste of vomit from the mouth. This causes even more harm to the teeth, as brushing your teeth over acidic gastric juices will increase the rate at which your teeth surfaces erode away.
- tooth decay and infection: teeth that has undergone erosion are more susceptible to caries attack and infection of the pulp.
What role does a dentist play?
A bulimic patient may not even realize that they have a problem other than they are innocently trying to “control their weightâ€. They are even more unlikely to admit to being a bulimic if confronted. There are no tell-tale signs other than the effects in the mouth and teeth, therefore a dentist possibly plays a frontline role in identifying a bulimic patient. A dentist should suspect bulimia if a patient comes to him with the following manifestations:
- a distinctive dental erosion pattern, especially on the lingual surfaces of upper front teeth. The dentist can also tell whether the patient is a chronic bulimic or a relatively recent one, from the degree of erosion on the teeth.
- Inflamed gums
- Enlarged salivary glands
- Dryness of mouth (xerostomia) and decreased saliva production or saliva flow – this is related to the use of laxatives and diuretics and dehydration from fasting and vomiting.
- redness and soreness of tongue, throat and the roof of the mouth (the palate)
- red, cracked and dry lips
- difficulty in swallowing
If bulimia is suspected, the dentist should first talk to the patient or the parents about it. The patient may not even be aware of the negative effects of their actions on their teeth, as the erosion may take years before it becomes prominent. Also, the lingual surfaces are affected first, which is unseen if the patient looks into a mirror. If the patient is willing, he or she can be referred to a psychiatrist, as this eating disorder involves a psychological behavior beyond health issues. The dentist should learn how to approach these patients with sensitivity and concern, as most patients will not be willing to talk about their eating disorder.
Treatment for teeth and mouth affected by bulimia
- regular professional dental cleaning procedures
- professional fluoride application and home application of fluoride
- use of artificial saliva
- for those who are still unable to stop self-induced vomiting, they should be advised to rinse their mouth with water or a fluoride rinse immediately following vomiting, and also never to brush their teeth immediately after vomiting.
- use of desensitizing toothpaste
- frequent dental visits to monitor the condition of the teeth and mouth.
- If the patient has successfully given up on the abnormal practice of binging and purging, teeth that has been damaged can be restored either with restorations, crown and bridges, dentures, or implants.