Extracting teeth may be one of the most commonly done procedures in a dental setting, but few are aware of the complications associated with the procedure. This is just to name some of them: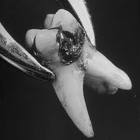
1. Soft tissue injury
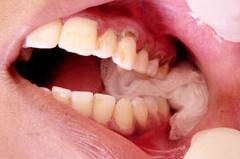
Pulling out a tooth requires a considerably big amount of force; if the dentist does not have a firm grip on his instruments on the tooth, there is a chance of slippage. All the surrounding soft tissues are subject to injury, i.e. the cheeks, tongue, lips, and even skin. Sometimes, an unsightly burnt mark may be left on the skin when the rotary part of a rotary instrument is unintentionally placed against the skin.
2. Injury to the tooth to be extracted
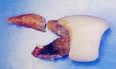
- A tooth with long, curved and thin roots or a tooth with an existing fracture line stand a higher chance of fracture. Another factor is when the dentist does not have a firm or deep enough grip on the tooth, the force of extraction is not transmitted to the entire tooth, but only to the crown (the part of the tooth visible in the human mouth). Hence the crown of the tooth is crushed while the root remains in its socket.
- In upper teeth, where the roots of the teeth are in close proximity to the maxillary sinus (behind the cheek bones), the fractured root may be displaced into the sinus wall. If the fractured remnant is but a small piece, it can be left intact, as it will fuse with the wall of the sinus and not cause any harm. However, if the fracture root is large, it should be removed.
3. Injury to adjacent tooth
- A dentist may require using the adjacent tooth as leverage during extraction, especially when extracting the back teeth. This exposes the adjacent tooth to the risk of coming loose, or fractured filling if there was a filling on that tooth.
- A dentist can make the unforgiveable mistake of extracting the wrong tooth! So make sure you know which tooth needs to be extracted, and get your dentist to show you the tooth he is about to extract with a mirror before he proceeds with it.
4. Fracture of bone
The dentist usually looses the attachment of the tooth to its socket (the periodontal ligament) before going about extracting the tooth. This serves also to create space so that the forceps can reach a deeper level of the root to enable a firm grip of the tooth. If this attachment is not severed, when the tooth is pulled out, the attachment may pull some about of bone with it as well, especially where the bone is thinner, eg the walls of the socket in lower front teeth.
5. Non-stop Bleeding
Following extraction, your dentist will often ask you to bite on a piece of gauze. This is to apply pressure to stop the bleeding. If after several minutes your wound is still bleeding profusely, it becomes a complication and other measures have to be taken. Therefore it is important that patients are asked about their medical history, whether they have a history of bleeding problems (e.g. prolonged bleeding after a minor cut anywhere on the body) or are taking any medications that may inhibit blood clot formation (e.g. aspirin) before proceeding with an extraction.
6. Damage to associated structures:
- The face and head is rich with nerve vessels, hence patients may suffer from nerve injury following extraction.
- If your jaw is not well-supported during an extraction, the force of extraction may be transmitted to your jaw joint, especially during extraction of lower back teeth which requires a larger amount of force.
7. Infective endocarditis (I.E.)
I.E. is the bacterial infection of the endocardial surface of the heart. In a dental setting, I.E. can occur when an invasive procedure is carried out, such as in an extraction. The bacteria from the mouth, particularly the staphylococcus aureus is then carried into the bloodstream, and eventually brought back to the heart, where it attaches to the wall of the heart and manifest as infective endocarditis. Only certain people at risk of I.E., eg people who have a prosthetic heart valve, a history of I.E. or certain congenital heart diseases.
8. Delayed healing and infection
- Poor healing of an extraction wound can lead to wound dehiscence, or the splitting of the wound. This can be avoided by the dentist by being careful and applying aseptic techniques.
- Infection of an extraction wound is fairly rare.
- Dry socket is a condition whereby wound healing is delayed. The socket becomes extremely painful, smelly and the patient will complain of a foul taste. The cause is unknown, but it is not associated with infection.